
PART FIVE PATHS TO RECOVERY
CHAPTER 13 HEALING FROM TRAUMA: OWNING YOUR SELF
I don’t go to therapy to find out if I’m a freak
I go and I find the one and only answer every week
And when I talk about therapy, I know what people think
When I finally got to talk so much about myself
—Dar Williams, What Do You Hear in These Sounds
Nobody can “treat” a war, or abuse, rape, molestation, or any event for that matter; what has happened cannot be undone.
But what can be dealt with are the imprints of the trauma on body, mind, and soul: the crushing sensations in your chest that you may label as anxiety or depression; the fear of losing control; always being on alert for danger or rejection; the self-loathing; the nightmares and flashbacks; the fog that keeps you from staying on task and from engaging fully in what you are doing; being unable to fully open your heart to another human being.
Trauma robs you of the feeling that you are in charge of yourself, of what I will call self-leadership in the chapters to come.1 The challenge of recovery is to reestablish ownership of your body and your mind—of your self. This means feeling free to know what you know and to feel what you feel without becoming overwhelmed, enraged, ashamed, or collapsed.
These goals are not steps to be achieved, one by one, in some fixed sequence. They overlap, and some may be more difficult than others, depending on individual circumstances.
I have done scientific studies of many of the treatments I describe here and have published the research findings in peer-reviewed scientific journals.2
A NEW FOCUS FOR RECOVERY
When we talk about trauma, we often start with a story or a question: “What happened during the war?” “Were you ever molested?” “Let me tell you about that accident or that rape,” or “Was anybody in your family a problem drinker?”
In order to regain control over your self, you need to revisit the trauma: Sooner or later you need to confront what has happened to you, but only after you feel safe and will not be retraumatized by it.
As the previous parts of this book have shown, the engines of posttraumatic reactions are located in the emotional brain.
Why can’t we just be reasonable? And can understanding help? The rational, executive brain is good at helping us understand where feelings come from (as in: “I get scared when I get close to a guy because my father molested me” or “I have trouble expressing my love toward my son because I feel guilty about having killed a child in Iraq”).
LIMBIC SYSTEM THERAPY
The fundamental issue in resolving traumatic stress is to restore the proper balance between the rational and emotional brains, so that you can feel in charge of how you respond and how you conduct your life.
As long as people are either hyperaroused or shut down, they cannot learn from experience. Even if they manage to stay in control, they become so uptight (Alcoholics Anonymous calls this “white-knuckle sobriety”) that they are inflexible, stubborn, and depressed.
If we want to change posttraumatic reactions, we have to access the emotional brain and do “limbic system therapy”:
- repairing faulty alarm systems and
- restoring the emotional brain to its ordinary job of being a quiet background presence that takes care of the housekeeping of the body,
- ensuring that you eat, sleep, connect with intimate partners, protect your children, and defend against danger.
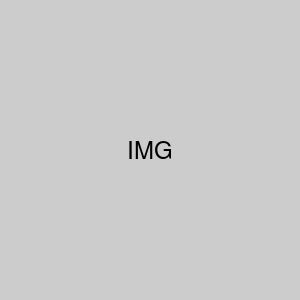
DRAWING BY LICIA SKY
Accessing the emotional brain. The rational, analyzing part of the brain, centered on the dorsolateral prefrontal cortex, has no direct connections with the emotional brain, where most imprints of trauma reside, but the medial prefrontal cortex, the center of self-awareness, does.
The neuroscientist Joseph LeDoux and his colleagues have shown that the only way we can consciously access the emotional brain is through self-awareness, i.e. by activating the medial prefrontal cortex, the part of the brain that notices what is going on inside us and thus allows us to feel what we’re feeling.5 (The technical term for this is “interoception”—Latin for “looking inside.”)
BEFRIENDING THE EMOTIONAL BRAIN
1. DEALING WITH HYPERAROUSAL
Over the past few decades mainstream psychiatry has focused on using drugs to change the way we feel, and this has become the accepted way to deal with hyper-and hypoarousal. I will discuss drugs later in this chapter, but first I need to stress the fact that we have a host of inbuilt skills to keep us on an even keel. In chapter 5 we saw how emotions are registered in the body. Some 80 percent of the fibers of the vagus nerve (which connects the brain with many internal organs) are afferent; that is, they run from the body into the brain.6 This means that we can directly train our arousal system by the way we breathe, chant, and move, a principle that has been utilized since time immemorial in places like China and India, and in every religious practice that I know of, but that is suspiciously eyed as “alternative” in mainstream culture.
In research supported by the National Institutes of Health, my colleagues and I have shown that ten weeks of yoga practice markedly reduced the PTSD symptoms of patients who had failed to respond to any medication or to any other treatment.7 (I will discuss yoga in chapter 16.) Neurofeedback, the topic of chapter 19, also can be particularly effective for children and adults who are so hyperaroused or shut down that they have trouble focusing and prioritizing.8
Learning how to breathe calmly and remaining in a state of relative physical relaxation, even while accessing painful and horrifying memories, is an essential tool for recovery.9 When you deliberately take a few slow, deep breaths, you will notice the effects of the parasympathetic brake on your arousal (as explained in chapter 5). The more you stay focused on your breathing, the more you will benefit, particularly if you pay attention until the very end of the out breath and then wait a moment before you inhale again. As you continue to breathe and notice the air moving in and out of your lungs you may think about the role that oxygen plays in nourishing your body and bathing your tissues with the energy you need to feel alive and engaged. Chapter 16 documents the full-body effects of this simple practice.
Since emotional regulation is the critical issue in managing the effects of trauma and neglect, it would make an enormous difference if teachers, army sergeants, foster parents, and mental health professionals were thoroughly schooled in emotional-regulation techniques. Right now this still is mainly the domain of preschool and kindergarten teachers, who deal with immature brains and impulsive behavior on a daily basis and who are often very adept at managing them.10
Mainstream Western psychiatric and psychological healing traditions have paid scant attention to self-management. In contrast to the Western reliance on drugs and verbal therapies, other traditions from around the world rely on mindfulness, movement, rhythms, and action.
2. NO MIND WITHOUT MINDFULNESS
At the core of recovery is self-awareness.
Body awareness puts us in touch with our inner world, the landscape of our organism.
Traumatized people are often afraid of feeling.
In order to change you need to open yourself to your inner experience.
“Focus on that sensation andsee how it changes when you take a deep breath out,or when you tap your chest just below your collarbone,or when you allow yourself to cry.”
We can tolerate a great deal discomfort as long as we stay conscious of the fact that the body’s commotions constantly shift. One moment your chest tightens, but after you take a deep breath and exhale, that feeling softens and you may observe something else, perhaps a tension in your shoulder. Now you can start exploring what happens when you take a deeper breath and notice how your rib cage expands.13 Once you feel calmer and more curious, you can go back to that sensation in your shoulder. You should not be surprised if a memory spontaneously arises in which that shoulder was somehow involved.
A further step is to observe the interplay between your thoughts and your physical sensations. How are particular thoughts registered in your body? (Do thoughts like “My father loves me” or “my girlfriend dumped me” produce different sensations?) Becoming aware of how your body organizes particular emotions or memories opens up the possibility of releasing sensations and impulses you once blocked in order to survive.14 In chapter 20, on the benefits of theater, I’ll describe in more detail how this works.
Jon Kabat-Zinn, one of the pioneers in mind-body medicine, founded the Mindfulness-Based Stress Reduction (MBSR) program at the University of Massachusetts Medical Center in 1979, and his method has been thoroughly studied for more than three decades.
Mindfulness has been shown to have a positive effect on numerous psychiatric, psychosomatic, and stress-related symptoms, including depression and chronic pain.16
3. RELATIONSHIPS
Study after study shows that having a good support network constitutes the single most powerful protection against becoming traumatized.
After an acute trauma, like an assault, accident, or natural disaster, survivors require the presence of familiar people, faces, and voices; physical contact; food; shelter and a safe place; and time to sleep. It is critical to communicate with loved ones close and far and to reunite as soon as possible with family and friends in a place that feels safe. Our attachment bonds are our greatest protection against threat. For example, children who are separated from their parents after a traumatic event are likely to suffer serious negative long-term effects. Studies conducted during World War II in England showed that children who lived in London during the Blitz and were sent away to the countryside for protection against German bombing raids fared much worse than children who remained with their parents and endured nights in bomb shelters and frightening images of destroyed buildings and dead people.21
Traumatized human beings recover in the context of relationships: with families, loved ones, AA meetings, veterans’ organizations, religious communities, or professional therapists. The role of those relationships is to provide physical and emotional safety, including safety from feeling shamed, admonished, or judged, and to bolster the courage to tolerate, face, and process the reality of what has happened.
As we have seen, much the wiring of our brain circuits is devoted to being in tune with others. Recovery from trauma involves (re)connecting with our fellow human beings. This is why trauma that has occurred within relationships is generally more difficult to treat than trauma resulting from traffic accidents or natural disasters. In our society the most common traumas in women and children occur at the hands of their parents or intimate partners. Child abuse, molestation, and domestic violence all are inflicted by people who are supposed to love you. That knocks out the most important protection against being traumatized: being sheltered by the people you love.
If the people whom you naturally turn to for care and protection terrify or reject you, you learn to shut down and to ignore what you feel.22 As we saw in part 3, when your caregivers turn on you, you have to find alternative ways to deal with feeling scared, angry, or frustrated. Managing your terror all by yourself gives rise to another set of problems: dissociation, despair, addictions, a chronic sense of panic, and relationships that are marked by alienation, disconnection, and explosions. Patients with these histories rarely make the connection between what happened to them long ago and how they currently feel and behave. Everything just seems unmanageable.
Relief does not come until they are able to acknowledge what has happened and recognize the invisible demons they’re struggling with. Recall, for example, the men I described in chapter 11 who had been abused by pedophile priests. They visited the gym regularly, took anabolic steroids, and were strong as oxen. However, in our interviews they often acted like scared kids; the hurt boys deep inside still felt helpless.
While human contact and attunement are the wellspring of physiological self-regulation, the promise of closeness often evokes fear of getting hurt, betrayed, and abandoned. Shame plays an important role in this: “You will find out how rotten and disgusting I am and dump me as soon as you really get to know me.” Unresolved trauma can take a terrible toll on relationships. If your heart is still broken because you were assaulted by someone you loved, you are likely to be preoccupied with not getting hurt again and fear opening up to someone new. In fact, you may unwittingly try to hurt them before they have a chance to hurt you.
This poses a real challenge for recovery. Once you recognize that posttraumatic reactions started off as efforts to save your life, you may gather the courage to face your inner music (or cacophony), but you will need help to do so. You have to find someone you can trust enough to accompany you, someone who can safely hold your feelings and help you listen to the painful messages from your emotional brain. You need a guide who is not afraid of your terror and who can contain your darkest rage, someone who can safeguard the wholeness of you while you explore the fragmented experiences that you had to keep secret from yourself for so long. Most traumatized individuals need an anchor and a great deal of coaching to do this work.
Choosing a Professional Therapist
The training of competent trauma therapists involves learning about the impact of trauma, abuse, and neglect and mastering a variety of techniques that can help to (1) stabilize and calm patients down,
While it’s inappropriate and unethical for therapists to tell you the details of their personal struggles, it is perfectly reasonable to ask what particular forms of therapy they have been trained in, where they learned their skills, and whether they’ve personally benefited from the therapy they propose for you.
There is no one “treatment of choice” for trauma, and any therapist who believes that his or her particular method is the only answer to your problems is suspect of being an ideologue rather than somebody who is interested in making sure that you get well. No therapist can possibly be familiar with every effective treatment, and he or she must be open to your exploring options other than the ones he or she offers. He or she also must be open to learning from you. Gender, race, and personal background are relevant only if they interfere with helping the patient feel safe and understood.
Do you feel basically comfortable with this therapist? Does he or she seem to feel comfortable in his or her own skin and with you as a fellow human being? Feeling safe is a necessary condition for you to confront your fears and anxieties. Someone who is stern, judgmental, agitated, or harsh is likely to leave you feeling scared, abandoned, and humiliated, and that won’t help you resolve your
traumatic stress. There may be times as old feelings from the past are stirred up, when you become suspicious that the therapist resembles someone who once hurt or abused you. Hopefully, this is something you can work through together, because in my experience patients get better only if they develop deep positive feelings for their therapists. I also don’t think that you can grow and change unless you feel that you have some impact on the person who is treating you.
The critical question is this: Do you feel that your therapist is curious to find out who you are and what you, not some generic “PTSD patient,” need? Are you just a list of symptoms on some diagnostic questionnaire, or does your therapist take the time to find out why you do what you do and think what you think? Therapy is a collaborative process—a mutual exploration of your self.
Patients who have been brutalized by their caregivers as children often do not feel safe with anyone. I often ask my patients if they can think of any person they felt safe with while they were growing up. Many of them hold tight to the memory of that one teacher, neighbor, shopkeeper, coach, or minister who showed that he or she cared, and that memory is often the seed of learning to reengage. We are a hopeful species. Working with trauma is as much about remembering how we survived as it is about what is broken.
I also ask my patients to imagine what they were like as newborns—whether they were lovable and filled with spunk. All of them believe they were and have some image of what they must have been like before they were hurt.
Some people don’t remember anybody they felt safe with. For them, engaging with horses or dogs may be much safer than dealing with human beings. This principle is currently being applied in many therapeutic settings to great effect, including in jails, residential treatment programs, and veterans’ rehabilitation. Jennifer, a member of the first graduating class of the Van der Kolk Center,23 who had come to the program as an out-of-control, mute fourteen-year-old, said during her graduation ceremony that having been entrusted with the responsibility of caring for a horse was the critical first step for her. Her growing bond with her horse helped her feel safe enough to begin to relate to the staff of the center and then to focus on her classes, take her SATs, and be accepted to college.24
4. COMMUNAL RHYTHMS AND SYNCHRONY
From the moment of our birth, our relationships are embodied in responsive faces, gestures, and touch. As we saw in chapter 7, these are the foundations of
attachment. Trauma results in a breakdown of attuned physical synchrony: When you enter the waiting room of a PTSD clinic, you can immediately tell the patients from the staff by their frozen faces and collapsed (but simultaneously agitated) bodies. Unfortunately, many therapists ignore those physical communications and focus only on the words with which their patients communicate.
The healing power of community as expressed in music and rhythms was brought home for me in the spring of 1997, when I was following the work of the Truth and Reconciliation Commission in South Africa. In some places we visited, terrible violence continued. One day I attended a group for rape survivors in the courtyard of a clinic in a township outside Johannesburg. We could hear the sound of bullets being fired at a distance while smoke billowed over the walls of the compound and the smell of teargas hung in the air. Later we heard that forty people had been killed.
Yet, while the surroundings were foreign and terrifying, I recognized this group all too well: The women sat slumped over—sad and frozen—like so many rape therapy groups I had seen in Boston. I felt a familiar sense of helplessness, and, surrounded by collapsed people, I felt myself mentally collapse as well. Then one of the women started to hum, while gently swaying back and forth. Slowly a rhythm emerged; bit by bit other women joined in. Soon the whole group was singing, moving, and getting up to dance. It was an astounding transformation: people coming back to life, faces becoming attuned, vitality returning to bodies. I made a vow to apply what I was seeing there and to study how rhythm, chanting, and movement can help to heal trauma.
We will see more of this in chapter 20, on theater, where I show how groups of young people—among them juvenile offenders and at-risk foster kids— gradually learn to work together and to depend on one another, whether as partners in Shakespearean swordplay or as the writers and performers of full-length musicals. Different patients have told me how much choral singing, aikido, tango dancing, and kickboxing have helped them, and I am delighted to pass their recommendations on to other people I treat.
I learned another powerful lesson about rhythm and healing when clinicians at the Trauma Center were asked to treat a five-year-old mute girl, Ying Mee, who had been adopted from an orphanage in China. After months of failed attempts to make contact with her, my colleagues Deborah Rozelle and Liz Warner realized that her rhythmical engagement system didn’t work—she could not resonate with the voices and faces of the people around her. That led them to sensorimotor therapy.25
The sensory integration clinic in Watertown, Massachusetts, is a wondrous indoor playground filled with swings, tubs full of multicolored rubber balls so deep that you can make yourself disappear, balance beams, crawl spaces fashioned from plastic tubing, and ladders that lead to platforms from which you can dive onto foam-filled mats. The staff bathed Ying Mee in the tub with plastic balls; that helped her feel sensations on her skin. They helped her sway on swings and crawl under weighted blankets. After six weeks something shifted —and she started to talk.26
Ying Mee’s dramatic improvement inspired us to start a sensory integration clinic at the Trauma Center, which we now also use in our residential treatment programs. We have not yet explored how well sensory integration works for traumatized adults, but I regularly incorporate sensory integration experiences and dance in my seminars.
Learning to become attuned provides parents (and their kids) with the visceral experience of reciprocity. Parent-child interaction therapy (PCIT) is an interactive therapy that fosters this, as is SMART (sensory motor arousal regulation treatment), developed by my colleagues at the Trauma Center.27
When we play together, we feel physically attuned and experience a sense of connection and joy. Improvisation exercises (such as those found at http://learnimprov.com/) also are a marvelous way to help people connect in joy and exploration. The moment you see a group of grim-faced people break out in a giggle, you know that the spell of misery has broken.
5. GETTING IN TOUCH
Mainstream trauma treatment has paid scant attention to helping terrified people to safely experience their sensations and emotions. Medications such as serotonin reuptake blockers, Respiridol and Seroquel increasingly have taken the place of helping people to deal with their sensory world.28 However, the most natural way that we humans calm down our distress is by being touched, hugged, and rocked. This helps with excessive arousal and makes us feel intact, safe, protected, and in charge.
Rembrandt van Rijn: Christ Healing the Sick. Gestures of comfort are universally recognizable and reflect the healing power of attuned touch.
Touch, the most elementary tool that we have to calm down, is proscribed from most therapeutic practices. Yet you can’t fully recover if you don’t feel safe in your skin. Therefore, I encourage all my patients to engage in some sort of bodywork, be it therapeutic massage, Feldenkrais, or craniosacral therapy.
I asked my favorite bodywork practitioner, Licia Sky, about her practice with traumatized individuals. Here is some of what she told me: “I never begin a bodywork session without establishing a personal connection. I’m not taking a history; I’m not finding out how traumatized a person is or what happened to them. I check in where they are in their body right now. I ask them if there is anything they want me to pay attention to. All the while, I’m assessing their posture; whether they look me in the eye; how tense or relaxed they seem; are they connecting with me or not.
“The first decision I make is if they will feel safer face up or face down. If I don’t know them, I usually start face up. I am very careful about draping; very careful to let them feel safe with whatever clothing they want to leave on. These are important boundaries to set up right at the beginning.
“Then, with my first touch, I make firm, safe contact. Nothing forced or sharp. Nothing too fast. The touch is slow, easy for the client to follow, gently rhythmic. It can be as strong as a handshake. The first place I might touch is their hand and forearm, because that’s the safest place to touch anybody, the place where they can touch you back.
“You have to meet their point of resistance—the place that has the most tension—and meet it with an equal amount of energy. That releases the frozen tension. You can’t hesitate; hesitation communicates a lack of trust in yourself. Slow movement, careful attuning to the client is different from hesitation. You have to meet them with tremendous confidence and empathy, let the pressure of your touch meet the tension they are holding in their bodies.”
What does bodywork do for people? Licia’s reply: “Just like you can thirst for water, you can thirst for touch. It is a comfort to be met confidently, deeply, firmly, gently, responsively. Mindful touch and movement grounds people and allows them to discover tensions that they may have held for so long that they are no longer even aware of them. When you are touched, you wake up to the part of your body that is being touched.
“The body is physically restricted when emotions are bound up inside. People’s shoulders tighten; their facial muscles tense. They spend enormous energy on holding back their tears—or any sound or movement that might betray their inner state. When the physical tension is released, the feelings can be released. Movement helps breathing to become deeper, and as the tensions are released, expressive sounds can be discharged. The body becomes freer— breathing freer, being in flow. Touch makes it possible to live in a body that can move in response to being moved.
“People who are terrified need to get a sense of where their bodies are in space and of their boundaries. Firm and reassuring touch lets them know where those boundaries are: what’s outside them, where their bodies end. They discover that they don’t constantly have to wonder who and where they are. They discover that their body is solid and that they don’t have to be constantly on guard. Touch lets them know that they are safe.”
6. TAKING ACTION
The body responds to extreme experiences by secreting stress hormones. These are often blamed for subsequent illness and disease.
Helplessness and immobilization keep people from utilizing their stress hormones to defend themselves. When that happens, their hormones still are being pumped out, but the actions they’re supposed to fuel are thwarted. Eventually, the activation patterns that were meant to promote coping are turned back against the organism and now keep fueling inappropriate fight/flight and freeze responses. In order to return to proper functioning, this persistent emergency response must come to an end. The body needs to be restored to a baseline state of safety and relaxation from which it can mobilize to take action in response to real danger.
My friends and teachers Pat Ogden and Peter Levine have each developed powerful body-based therapies, sensorimotor psychotherapy29 and somatic experiencing30 to deal with this issue. In these treatment approaches the story of what has happened takes a backseat to exploring physical sensations and discovering the location and shape of the imprints of past trauma on the body. Before plunging into a full-fledged exploration of the trauma itself, patients are helped to build up internal resources that foster safe access sensations and emotions that overwhelmed them at the time of the trauma. Peter Levine calls this process pendulation—gently moving in and out of accessing internal sensations and traumatic memories. In this way patients are helped to gradually expand their window of tolerance.
Once patients can tolerate being aware of their trauma-based physical experiences, they are likely to discover powerful physical impulses—like hitting, pushing, or running—that arose during the trauma but were suppressed in order to survive. These impulses manifest themselves in subtle body movements such as twisting, turning, or backing away. Amplifying these movements and experimenting with ways to modify them begins the process of bringing the incomplete, trauma-related “action tendencies” to completion and can eventually lead to resolution of the trauma. Somatic therapies can help patients to relocate themselves in the present by experiencing that it is safe to move. Feeling the pleasure of taking effective action restores a sense of agency and a sense of being able to actively defend and protect themselves.
Back in 1893 Pierre Janet, the first great explorer of trauma, wrote about “the pleasure of completed action,” and I regularly observe that pleasure when I practice sensorimotor psychotherapy and somatic experiencing:
When people are forced to submit to overwhelming power, as is true for most abused children, women trapped in domestic violence, and incarcerated men and women,
One of my patients, a college student with a history of unrelenting child abuse, took the course. When I first met her, she was collapsed, depressed, and overly compliant. Three months later, during her graduation ceremony, she successfully fought off a gigantic male attacker who ended up lying cringing on the floor (shielded from her blows by a thick protective suit) while she faced him, arms raised in a karate stance, calmly and clearly yelling no.
Not long afterward, she was walking home from the library after midnight when three men jumped out of some bushes, yelling: “Bitch, give us your money.” She later told me that she took that same karate stance and yelled back: “Okay, guys, I’ve been looking forward to this moment. Who wants to take me on first?” They ran away. If you’re hunched over and too afraid to look around, you are easy prey to other people’s sadism, but when you walk around projecting the message “Don’t mess with me,” you’re not likely to be bothered.
INTEGRATING TRAUMATIC MEMORIES
People cannot put traumatic events behind until they are able to acknowledge what has happened and start to recognize the invisible demons they’re struggling with.
There is a reason for that. When people remember an ordinary event, they do not also relive the physical sensations, emotions, images, smells, or sounds associated with that event.
A trauma can be successfully processed only if all those brain structures are kept online. In Stan’s case, eye movement desensitization and reprocessing (EMDR) allowed him to access his memories of the accident without being overwhelmed by them. When the brain areas whose absence is responsible for flashbacks can be kept online while remembering what has happened, people can integrate their traumatic memories as belonging to the past.
Ute’s dissociation (as you recall, she shut down completely) complicated recovery in a different way. None of the brain structures necessary to engage in the present were online, so that dealing with the trauma was simply impossible. Without a brain that is alert and present there can be no integration and resolution. She needed to be helped to increase her window of tolerance before she could deal with her PTSD symptoms.
Hypnosis was the most widely practiced treatment for trauma from the late 1800s, the time of Pierre Janet and Sigmund Freud, until after World War II. On YouTube you can still watch the documentary Let There Be Light, by the great Hollywood director John Huston, which shows men undergoing hypnosis to treat “war neurosis.” Hypnosis fell out of favor in the early 1990s and there have been no recent studies of its effectiveness for treating PTSD. However, hypnosis can induce a state of relative calm from which patients can observe their traumatic experiences without being overwhelmed by them. Since that capacity to quietly observe oneself is a critical factor in the integration of traumatic memories, it is likely that hypnosis, in some form, will make a comeback.
COGNITIVE BEHAVIORAL THERAPY (CBT) 인지 행동 치료
During their training most psychologists are taught cognitive behavioral therapy. CBT was first developed to treat phobias such as fear of spiders, airplanes, or heights, to help patients compare their irrational fears with harmless realities. Patients are gradually desensitized from their irrational fears by bringing to mind what they are most afraid of, using their narratives and images (“imaginal exposure”), or they are placed in actual (but actually safe) anxiety-provoking situations (“in vivo exposure”), or they are exposed to virtual-reality, computer-simulated scenes, for example, in the case of combat-related PTSD, fighting in the streets of Fallujah.
The idea behind cognitive behavioral treatment is that when patients are repeatedly exposed to the stimulus without bad things actually happening, they gradually will become less upset; the bad memories will have become associated with “corrective” information of being safe.33 CBT also tries to help patients deal with their tendency to avoid, as in “I don’t want to talk about it.”34 It sounds simple, but, as we have seen, reliving trauma reactivates the brain’s alarm system and knocks out critical brain areas necessary for integrating the past, making it likely that patients will relive rather than resolve the trauma.
Prolonged exposure or “flooding” has been studied more thoroughly than any other PTSD treatment. Patients are asked to “focus their attention on the traumatic material and. . . not distract themselves with other thoughts or activities.”35 Research has shown that up to one hundred minutes of flooding (in which anxiety-provoking triggers are presented in an intense, sustained form) are required before decreases in anxiety are reported.36 Exposure sometimes helps to deal with fear and anxiety, but it has not been proven to help with guilt or other complex emotions.37
In contrast to its effectiveness for irrational fears such as spiders, CBT has not done so well for traumatized individuals, particularly those with histories of childhood abuse. Only about one in three participants with PTSD who finish research studies show some improvement.38 Those who complete CBT treatment usually have fewer PTSD symptoms, but they rarely recover completely: Most continue to have substantial problems with their health, work, or mental well-being.39
In the largest published study of CBT for PTSD more than one-third of the patients dropped out; the rest had a significant number of adverse reactions. Most of the women in the study still suffered from full-blown PTSD after three months in the study, and only 15 percent no longer had major PTSD symptoms.40 A thorough analysis of all the scientific studies of CBT show that it works about as well as being in a supportive therapy relationship.41 The poorest outcome in exposure treatments occurs in patients who suffer from “mental defeat”—those who have given up.42
Being traumatized is not just an issue of being stuck in the past; it is just as much a problem of not being fully alive in the present. One form of exposure treatment is virtual-reality therapy in which veterans wear high-tech goggles that make it possible to refight the battle of Fallujah in lifelike detail. As far as I know, the US Marines performed very well in combat. The problem is that they cannot tolerate being home. Recent studies of Australian combat veterans show that their brains are rewired to be alert for emergencies, at the expense of being focused on the small details of everyday life.43 (We’ll learn more about this in chapter 19, on neurofeedback.) More than virtual-reality therapy, traumatized patients need “real world” therapy, which helps them to feel as alive when walking through the local supermarket or playing with their kids as they did in the streets of Baghdad.
Patients can benefit from reliving their trauma only if they are not overwhelmed by it. A good example is a study of Vietnam veterans conducted in the early 1990s by my colleague Roger Pitman.44 I visited Roger’s lab every week during that time, since we were conducting the study of brain opioids in PTSD that I discussed in chapter 2. Roger would show me the videotapes of his treatment sessions and we would discuss what we observed. He and his colleagues pushed the veterans to talk repeatedly about every detail of their experiences in Vietnam, but the investigators had to stop the study because many patients became panicked by their flashbacks, and the dread often persisted after the sessions. Some never returned, while many of those who stayed with the study became more depressed, violent, and fearful; some coped with their increased symptoms by increasing their alcohol consumption, which led to further violence and humiliation, as some of their families called the police to take them to a hospital.
DESENSITIZATION
Over the past two decades the prevailing treatment taught to psychology students has been some form of systematic desensitization: helping patients become less reactive to certain emotions and sensations. But is this the correct goal? Maybe the issue is not desensitization but integration: putting the traumatic event into its proper place in the overall arc of one’s life.
Desensitization makes me think of the small boy—he must have been about five—I saw in front of my house recently. His hulking father was yelling at him at the top of his voice as the boy rode his tricycle down my street. The kid was unfazed, while my heart was racing and I felt an impulse to deck the guy. How much brutality had it taken to numb a child this young to his father’s brutality? His indifference to his father’s yelling must have been the result of prolonged exposure, but, I wondered, at what price? Yes, we can take drugs that blunt our emotions or we can learn to desensitize ourselves. As medical students we learned to stay analytical when we had to treat children with third-degree burns. But, as the neuroscientist Jean Decety at the University of Chicago has shown, desensitization to our own or to other people’s pain tends to lead to an overall blunting of emotional sensitivity.45
A 2010 report on 49,425 veterans with newly diagnosed PTSD from the Iraq and Afghanistan wars who sought care from the VA showed that fewer than one out of ten actually completed the recommended treatment.46 As in Pitman’s Vietnam veterans, exposure treatment, as currently practiced, rarely works for them. We can only “process” horrendous experiences if they do not overwhelm us. And that means that other approaches are necessary.
DRUGS TO SAFELY ACCESS TRAUMA?
When I was a medical student, I spent the summer of 1966 working for Jan Bastiaans, a professor at Leiden University in the Netherlands who was known for his work treating Holocaust survivors with LSD. He claimed to have achieved spectacular results, but when colleagues inspected his archives, they found few data to support his claims. The potential of mind-altering substances for trauma treatment was subsequently neglected until 2000, when Michael Mithoefer and his colleagues in South Carolina received FDA permission to conduct an experiment with MDMA (ecstasy). MDMA was classified as a controlled substance in 1985 after having been used for years as a recreational drug. As with Prozac and other psychotropic agents, we don’t know exactly how MDMA works, but it is known to increase concentrations of a number of important hormones including oxytocin, vasopressin, cortisol, and prolactin.47 Most relevant for trauma treatment, it increases people’s awareness of themselves; they frequently report a heightened sense of compassionate energy, accompanied by curiosity, clarity, confidence, creativity, and connectedness. Mithoefer and his colleagues were looking for a medication that would enhance the effectiveness of psychotherapy, and they became interested in MDMA because it decreases fear, defensiveness, and numbing, as well as helping to access inner experience.48 They thought MDMA might enable patients to stay within the window of tolerance so they could revisit their traumatic memories without suffering overwhelming physiological and emotional arousal.
The initial pilot studies have supported that expectation.49 The first study, involving combat veterans, firefighters, and police officers with PTSD, had positive results. In the next study, of a group of twenty victims of assault who had been unresponsive to previous forms of therapy, twelve subjects received MDMA and eight received an inactive placebo. Sitting or lying in a comfortable room, they then all received two eight-hour psychotherapy sessions, mainly using internal family systems (IFS) therapy, the subject of chapter 17 of this book. Two months later 83 percent of the patients who received MDMA plus psychotherapy were considered completely cured, compared with 25 percent of the placebo group. None of the patients had adverse side effects. Perhaps most interesting, when the participants were interviewed more than a year after the study was completed, they had maintained their gains.
By being able to observe the trauma from the calm, mindful state that IFS calls Self (a term I’ll discuss further in chapter 17), mind and brain are in a position to integrate the trauma into the overall fabric of life. This is very different from traditional desensitization techniques, which are about blunting a person’s response to past horrors. This is about association and integration— making a horrendous event that overwhelmed you in the past into a memory of something that happened a long time ago.
Nonetheless, psychedelic substances are powerful agents with a troubled history. They can easily be misused through careless administration and poor maintenance of therapeutic boundaries. It is to be hoped that MDMA will not be another magic cure released from Pandora’s box.
WHAT ABOUT MEDICATIONS?
People have always used drugs to deal with traumatic stress. Each culture and each generation has its preferences—gin, vodka, beer, or whiskey; hashish, marijuana, cannabis, or ganja; cocaine; opioids like oxycontin; tranquilizers such as Valium, Xanax, and Klonopin. When people are desperate, they will do just about anything to feel calmer and more in control.50
Mainstream psychiatry follows this tradition. Over the past decade the Departments of Defense and Veterans Affairs combined have spent over $4.5 billion on antidepressants, antipsychotics, and antianxiety drugs. A June 2010 internal report from the Defense Department’s Pharmacoeconomic Center at Fort Sam Houston in San Antonio showed that 213,972, or 20 percent of the 1.1 million active-duty troops surveyed, were taking some form of psychotropic drug: antidepressants, antipsychotics, sedative hypnotics, or other controlled substances.51
However, drugs cannot “cure” trauma; they can only dampen the expressions of a disturbed physiology. And they do not teach the lasting lessons of self-regulation. They can help to control feelings and behavior, but always at a price—because they work by blocking the chemical systems that regulate engagement, motivation, pain, and pleasure. Some of my colleagues remain optimistic: I keep attending meetings where serious scientists discuss their quest for the elusive magic bullet that will miraculously reset the fear circuits of the brain (as if traumatic stress involved only one simple brain circuit). I also regularly prescribe medications.
Just about every group of psychotropic agents has been used to treat some aspect of PTSD.52 The serotonin reuptake inhibitors (SSRIs) such as Prozac, Zoloft, Effexor, and Paxil have been most thoroughly studied, and they can make feelings less intense and life more manageable. Patients on SSRIs often feel calmer and more in control; feeling less overwhelmed often makes it easier to engage in therapy. Other patients feel blunted by SSRIs—they feel they’re “losing their edge.” I approach it as an empirical question: Let’s see what works, and only the patient can be the judge of that. On the other hand, if one SSRI does not work, it’s worth trying another, because they all have slightly different effects. It’s interesting that the SSRIs are widely used to treat depression, but in a study in which we compared Prozac with eye movement desensitization and reprocessing (EMDR) for patients with PTSD, many of whom were also depressed, EMDR proved to be a more effective antidepressant than Prozac.53 I’ll return to that subject in chapter 15.54
Medicines that target the autonomic nervous system, like propranolol or clonidine, can help to decrease hyperarousal and reactivity to stress.55 This family of drugs works by blocking the physical effects of adrenaline, the fuel of arousal, and thus reduces nightmares, insomnia, and reactivity to trauma triggers.56 Blocking adrenaline can help to keep the rational brain online and make choices possible: “Is this really what I want to do?” Since I have started to integrate mindfulness and yoga into my practice, I use these medications less often, except occasionally to help patients sleep more restfully.
Traumatized patients tend to like tranquilizing drugs, benzodiazepines like Klonopin, Valium, Xanax, and Ativan. In many ways, they work like alcohol, in that they make people feel calm and keep them from worrying. (Casino owners love customers on benzodiazepines; they don’t get upset when they lose and keep gambling.) But also, like alcohol, benzos weaken inhibitions against saying hurtful things to people we love. Most civilian doctors are reluctant to prescribe these drugs, because they have a high addiction potential and they may also interfere with trauma processing. Patients who stop taking them after prolonged use usually have withdrawal reactions that make them agitated and increase posttraumatic symptoms.
I sometimes give my patients low doses of benzodiazepines to use as needed, but not enough to take on a daily basis. They have to choose when to use up their precious supply, and I ask them to keep a diary of what was going on when they decided to take the pill. That gives us a chance to discuss the specific incidents that triggered them.
A few studies have shown that anticonvulsants and mood stabilizers, such as lithium or valproate, can have mildly positive effects, taking the edge off hyperarousal and panic.57 The most controversial medications are the so-called second-generation antipsychotic agents, such as Risperdal and Seroquel, the largest-selling psychiatric drugs in the United States ($14.6 billion in 2008). Low doses of these agents can be helpful in calming down combat veterans and women with PTSD related to childhood abuse.58 Using these drugs is sometimes justified, for example when patients feel completely out of control and unable to sleep or where other methods have failed.59 But it’s important to keep in mind that these medications work by blocking the dopamine system, the brain’s reward system, which also functions as the engine of pleasure and motivation.
Antipsychotic medications such as Risperdal, Abilify, or Seroquel can significantly dampen the emotional brain and thus make patients less skittish or enraged, but they also may interfere with being able to appreciate subtle signals of pleasure, danger, or satisfaction. They also cause weight gain, increase the chance of developing diabetes, and make patients physically inert, which is likely to further increase their sense of alienation. These drugs are widely used to treat abused children who are inappropriately diagnosed with bipolar disorder or mood dysregulation disorder. More than half a million children and adolescents in America are now taking antipsychotic drugs, which may calm them down but also interfere with learning age-appropriate skills and developing friendships with other children.60 A Columbia University study recently found that prescriptions of antipsychotic drugs for privately insured two-to five-year-olds had doubled between 2000 and 2007.61 Only 40 percent of them had received a proper mental health assessment.
Until it lost its patent, the pharmaceutical company Johnson & Johnson doled out LEGO blocks stamped with the word “Risperdal” for the waiting rooms of child psychiatrists. Children from low-income families are four times as likely as the privately insured to receive antipsychotic medicines. In one year alone Texas Medicaid spent $96 million on antipsychotic drugs for teenagers and children—including three unidentified infants who were given the drugs before their first birthdays.62 There have been no studies on the effects of psychotropic medications on the developing brain. Dissociation, self-mutilation, fragmented memories, and amnesia generally do not respond to any of these medications.
The Prozac study that I discussed in chapter 2 was the first to discover that traumatized civilians tend to respond much better to medications than do combat veterans.63 Since then other studies have found similar discrepancies. In this light it is worrisome that the Department of Defense and the VA prescribe enormous quantities of medications to combat soldiers and returning veterans, often without providing other forms of therapy. Between 2001 and 2011 the VA spent about $1.5 billion on Seroquel and Risperdal, while Defense spent about $90 million during the same period, even though a research paper published in 2001 showed that Risperdal was no more effective than a placebo in treating PTSD.64 Similarly, between 2001 and 2012 the VA spent $72.1 million and Defense spent $44.1 million on benzodiazepines65—medications that clinicians generally avoid prescribing to civilians with PTSD because of their addiction potential and lack of significant effectiveness for PTSD symptoms.
THE ROAD OF RECOVERY IS THE ROAD OF LIFE
In the first chapter of this book I introduced you to a patient named Bill whom I met over thirty years ago at the VA. Bill became one of my longtime patient-teachers, and our relationship is also the story of my evolution of trauma treatment.
Bill had served as a medic in Vietnam in 1967–71, and after he returned, he tried to use the skills he had learned in the army by working on a burn unit in a local hospital. Nursing kept him frazzled, explosive, and on edge, but he had no idea that these problems had anything to do with what he had experienced in Vietnam. After all, the PTSD diagnosis did not yet exist, and Irish working-class guys in Boston didn’t consult shrinks. His nightmares and insomnia subsided a bit after he left nursing and enrolled in a seminary to become a minister. He did not seek help until after his first son was born in 1978.
The baby’s crying triggered unrelenting flashbacks, in which he saw, heard, and smelled burned and mutilated children in Vietnam. He was so out of control that some of my colleagues at the VA wanted to put him in the hospital to treat what they thought was a psychosis. However, as he and I started to work together and he began to feel safe with me, he gradually opened up about what he had witnessed in Vietnam, and he slowly started to tolerate his feelings without becoming overwhelmed. This helped him to refocus on taking care of his family and on finishing his training as a minister. After two years he was a pastor with his own parish, and we felt that our work was done.
I had no further contact with Bill until he called me up eighteen years to the day after I first met him. He was experiencing exactly the same symptoms— flashbacks, terrible nightmares, feelings that he was going crazy—that he’d had
right after his baby was born. That son had just turned eighteen, and Bill had accompanied him to register for the draft—at the same armory from which Bill himself had been shipped off to Vietnam. By then I knew much more about treating traumatic stress, and Bill and I dealt with the specific memories of what he had seen, heard, and smelled back in Vietnam, details that he had been too scared to recall when we first met. We could now integrate these memories with EMDR, so that they became stories of what happened long ago instead of instant transports into the hell of Vietnam. Once he felt more settled, he wanted to deal with his childhood: his brutal upbringing and his guilt about having left behind his younger schizophrenic brother when he enlisted for Vietnam, unprotected against their father’s violent outbursts.
Another important theme of our time together was the day-to-day pain Bill confronted as a minister—having to bury adolescents killed in car crashes only a few years after he’d baptized them or having couples he’d married come back in crisis over domestic violence. Bill went on to organize a support group for fellow clergy faced with similar traumas, and he became an important force in his community.
Bill’s third treatment started five years later, when he developed a serious neurological illness at age fifty-three. He had suddenly started to experience episodic paralysis in several parts of his body, and he was beginning to accept that he would probably spend the rest of his life in a wheelchair. I thought his problems might be due to multiple sclerosis, but his neurologists could not find specific lesions, and they said there was no cure for his condition. He told me how grateful he was for his wife’s support. She already had arranged to have a wheelchair ramp built to the kitchen entrance to their house.
Given his grim prognosis, I urged Bill to find a way to fully feel and befriend the distressing feelings in his body, just as he had learned to tolerate and live with his most painful memories of the war. I suggested that he consult a body worker who had introduced me to Feldenkrais, a gentle, hands-on approach to rearranging physical sensations and muscle movements.
Bill found a local Bikram yoga class, a hot and intense practice usually reserved for young and energetic people. Bill loved it, even though parts of his body occasionally gave way in class. Despite his physical disability, he gained a sense of bodily pleasure and mastery that he had never felt before.
Bill’s psychological treatment had helped him put the horrendous experience of Vietnam in the past. Now befriending his body was keeping him from organizing his life around the loss of physical control. He decided to become certified as a yoga instructor, and he began teaching yoga at his local armory to the veterans who were returning from Iraq and Afghanistan.
Today, ten years later, Bill continues to be fully engaged in life—with his children and grandchildren, through his work with veterans, and in his church. He copes with his physical limitations as an inconvenience. To date he has taught yoga classes to more than 1,300 returning combat veterans. He still regularly suffers from the sudden weakness in his limbs that requires him to sit or lie down. But, like his memories of childhood and Vietnam, these episodes do not dominate his existence. They are simply part of the ongoing, evolving story of his life.
CHAPTER 14 LANGUAGE: MIRACLE AND TYRANNY
Give sorrow words;
—William Shakespeare, Macbeth
We can hardly bear to look.
—Marion Woodman (as quoted by Stephen Cope in The Great Work of Your Life)
of
In September 2001 several organizations, including the National Institutes Health Pfizer pharmaceuticals and the New York Times Company Foundation, organized expert panels to recommend the best treatments for people traumatized by the attacks on the World Trade Center. Because many widely used trauma interventions had never been carefully evaluated in random communities (as opposed to patients who seek psychiatric help), I thought that this presented an extraordinary opportunity to compare how well a variety of different approaches would work. My colleagues were more conservative, and after lengthy deliberations the committees recommended only two forms of treatment: psychoanalytically oriented therapy and cognitive behavioral therapy. Why analytic talk therapy?
Dr. Spencer Eth, who ran the psychiatry department at the now-defunct St. Vincent’s Hospital in Greenwich Village, was curious where survivors had turned for help, and early in 2002, together with some medical students, he conducted a survey of 225 people who had escaped from the Twin Towers. Asked what had been most helpful in overcoming the effects of their experience, the survivors credited acupuncture, massage, yoga, and EMDR, in that order.1 Among rescue workers, massages were particularly popular. Eth’s survey suggests that the most helpful interventions focused on relieving the physical burdens generated by trauma. The disparity between the survivors’ experience and the experts’ recommendations is intriguing. Of course, we don’t know how many survivors eventually did seek out more traditional therapies. But the apparent lack of interest in talk therapy raises a basic question: What good is it to talk about your trauma?
THE UNSPEAKABLE TRUTH
Therapists have an undying faith in the capacity of talk to resolve trauma. That confidence dates back to 1893, when Freud (and his mentor, Breuer) wrote that trauma “immediately and permanently disappeared when we had succeeded in bringing clearly to light the memory of the event by which it was provoked and in arousing its accompanying affect, and when the patient had described that event in the greatest possible detail and had put the affect into words.”2
Unfortunately, it’s not so simple: Traumatic events are almost impossible to put into words. This is true for all of us, not just for people who suffer from PTSD. The initial imprints of the events of September 11 were not stories but images: frantic people running down the street, their faces covered with ash; an airplane smashing into Tower One of the World Trade Center; the distant specks that were people jumping hand in hand. Those images were replayed over and over, in our minds and on the TV screen, until Mayor Giuliani and the media helped us create a narrative we could share with one another.
In Seven Pillars of Wisdom T. E. Lawrence wrote of his war experiences: “We learned that there were pangs too sharp, griefs too deep, ecstasies too high for our finite selves to register. When emotion reached this pitch the mind choked; and memory went white till the circumstances were humdrum once more.”3 While trauma keeps us dumbfounded, the path out of it is paved with words, carefully assembled, piece by piece, until the whole story can be revealed.
BREAKING THE SILENCE
Activists in the early campaign for AIDS awareness created a powerful slogan: “Silence = Death.”
We may think we can control our grief, our terror, or our shame by remaining silent, but naming offers the possibility of a different kind of control. When Adam was put in charge of the animal kingdom in the Book of Genesis, his first act was to give a name to every living creature.
If you’ve been hurt, you need to acknowledge and name what happened to you. I know that from personal experience: As long as I had no place where I could let myself know what it was like when my father locked me in the cellar of our house for various three-year-old offenses, I was chronically preoccupied with being exiled and abandoned. Only when I could talk about how that little boy felt, only when I could forgive him for having been as scared and submissive as he was, did I start to enjoy the pleasure of my own company. Feeling listened to and understood changes our physiology; being able to articulate a complex feeling, and having our feelings recognized, lights up our limbic brain and creates an “aha moment.” In contrast, being met by silence and incomprehension kills the spirit. Or, as John Bowlby so memorably put it: “What can not be spoken to the [m]other cannot be told to the self.”
If you hide from yourself the fact that an uncle molested you when you were young, you are vulnerable to react to triggers like an animal in a thunderstorm: with a full-body response to the hormones that signal “danger.” Without language and context, your awareness may be limited to: “I’m scared.” Yet, determined to stay in control, you are likely to avoid anybody or anything that reminds you even vaguely of your trauma. You may also alternate between being inhibited and being uptight or reactive and explosive—all without knowing why.
As long as you keep secrets and suppress information, you are fundamentally at war with yourself. Hiding your core feelings takes an enormous amount of energy, it saps your motivation to pursue worthwhile goals, and it leaves you feeling bored and shut down. Meanwhile, stress hormones keep flooding your body, leading to headaches, muscle aches, problems with your bowels or sexual functions—and irrational behaviors that may embarrass you and hurt the people around you. Only after you identify the source of these responses can you start using your feelings as signals of problems that require your urgent attention.
Ignoring inner reality also eats away at your sense of self, identity, and purpose. Clinical psychologist Edna Foa and her colleagues developed the Posttraumatic Cognitions Inventory to assess how patients think about themselves.4 Symptoms of PTSD often include statements like “I feel dead inside,” “I will never be able to feel normal emotions again,” “I have permanently changed for the worse,” “I feel like an object, not like a person,” “I have no future,” and “I feel like I don’t know myself anymore.”
The critical issue is allowing yourself to know what you know. That takes an enormous amount of courage. In What It Is Like to Go to War, Vietnam veteran Karl Marlantes grapples with his memories of belonging to a brilliantly effective Marine combat unit and confronts the terrible split he discovered inside himself:
For years I was unaware of the need to heal that split, and there was no one, after I returned, to point this out to me.... Why did I assume there was only one person inside me? . . . There’s a part of me that just loves maiming, killing, and torturing. This part of me isn’t all of me. I have other elements that indeed are just the opposite, of which I am proud. So am I a killer? No, but part of me is. Am I a torturer? No, but part of me is. Do I feel horror and sadness when I read in the newspapers of an abused child? Yes. But am I fascinated?5
Marlantes tells us that his road to recovery required learning to tell the truth, even if that truth was brutally painful.
Death, destruction, and sorrow need to be constantly justified in the absence of some overarching meaning for the suffering. Lack of this overarching meaning encourages making things up, lying, to fill the gap in meaning.6
I’d never been able to tell anyone what was going on inside. So I forced these images back, away, for years. I began to reintegrate that split-off part of my experience only after I actually began to imagine that kid as a kid, my kid perhaps. Then, out came this overwhelming sadness—and healing. Integrating the feelings of sadness, rage, or all of the above with the action should be standard operating procedure for all soldiers who have killed face-to-face. It requires no sophisticated psychological training. Just form groups under a fellow squad or platoon member who has had a few days of group leadership training and encourage people to talk.7
Getting perspective on your terror and sharing it with others can reestablish the feeling that you are a member of the human race. After the Vietnam veterans I treated joined a therapy group where they could share the atrocities they had witnessed and committed, they reported beginning to open their hearts to their girlfriends.
THE MIRACLE OF SELF-DISCOVERY
Discovering your Self in language is always an epiphany, even if finding the words to describe your inner reality can be an agonizing process. That is why I find Helen Keller’s account of how she was “born into language”8 so inspiring.
When Helen was nineteen months old and just starting to talk, a viral infection robbed her of her sight and hearing. Now deaf, blind, and mute, this lovely, lively child turned into an untamed, isolated creature. After five desperate years her family invited a partially blind teacher, Anne Sullivan, to come from Boston to their home in rural Alabama as Helen’s tutor. Anne began immediately to teach Helen the manual alphabet, spelling words into her hand letter by letter, but it took ten weeks of trying to connect with this wild child before the breakthrough occurred. It came as Anne spelled the word “water” into one of Helen’s hands while she held the other under the water pump.
Helen later recalled that moment in The Story of My Life: “Water! That word startled my soul, and it awoke, full of the spirit of the morning. . . . Until that day
my mind had been like a darkened chamber, waiting for words to enter and light the lamp, which is thought. I learned a great many words that day.”
Learning the names of things enabled the child not only to create an inner representation of the invisible and inaudible physical reality around her but also to find herself: Six months later she started to use the first-person “I.”
Helen’s story reminds me of the abused, recalcitrant, uncommunicative kids we see in our residential treatment programs. Before she acquired language, she was bewildered and self-centered—looking back, she called that creature “Phantom.” And indeed, our kids come across as phantoms until they can discover who they are and feel safe enough to communicate what is going on with them.
In a later book, The World I Live In, Keller again described her birth into selfhood: “Before my teacher came to me, I did not know that I am. I lived in a world that was a no-world. . . . I had neither will nor intellect. . . . I can remember all this, not because I knew that it was so, but because I have tactual memory. It enables me to remember that I never contracted my forehead in the act of thinking.”9
Helen’s “tactual” memories—memories based only on touch—could not be shared. But language opened up the possibility of joining a community. At age eight, when Helen went with Anne to the Perkins Institution for the Blind in Boston (where Sullivan herself had trained), she became able to communicate with other children for the first time: “Oh, what happiness!” she wrote. “To talk freely with other children! To feel at home in the great world!”
Helen’s discovery of language with the help of Anne Sullivan captures the essence of a therapeutic relationship: finding words where words were absent before and, as a result, being able to share your deepest pain and deepest feelings with another human being. This is one of most profound experiences we can have, and such resonance, in which hitherto unspoken words can be discovered, uttered, and received, is fundamental to healing the isolation of trauma— especially if other people in our lives have ignored or silenced us. Communicating fully is the opposite of being traumatized.
KNOWING YOURSELF OR TELLING YOUR STORY? OUR DUAL AWARENESS SYSTEM
Anyone who enters talk therapy, however, almost immediately confronts the
limitations of language. This was true of my own psychoanalysis. While I talk easily and can tell interesting tales, I quickly realized how difficult it was to feel my feelings deeply and simultaneously report them to someone else. When I got in touch with the most intimate, painful, or confusing moments of my life, I often found myself faced with a choice: I could either focus on reliving old scenes in my mind’s eye and let myself feel what I had felt back then, or I could tell my analyst logically and coherently what had transpired. When I chose the latter, I would quickly lose touch with myself and start to focus on his opinion of what I was telling him. The slightest hint of doubt or judgment would shut me down, and I would shift my attention to regaining his approval.
Since then neuroscience research has shown that we possess two distinct forms of self-awareness: one that keeps track of the self across time and one that registers the self in the present moment. The first, our autobiographical self, creates connections among experiences and assembles them into a coherent story. This system is rooted in language. Our narratives change with the telling, as our perspective changes and as we incorporate new input.
The other system, moment-to-moment self-awareness, is based primarily in physical sensations, but if we feel safe are not rushed, we can find words to communicate that experience as well. These two ways of knowing are localized in different parts of the brain that are largely disconnected from each other.10 Only the system devoted to self-awareness, which is based in the medial prefrontal cortex, can change the emotional brain.
In the groups I used to lead for veterans, I could sometimes see these two systems working side by side. The soldiers told horrible tales of death and destruction, but I noticed that their bodies often simultaneously radiated a sense of pride and belonging. Similarly, many patients tell me about the happy families they grew up in while their bodies are slumped over and their voices sound anxious and uptight. One system creates a story for public consumption, and if we tell that story often enough, we are likely to start believing that it contains the whole truth. But the other system registers a different truth: how we experience the situation deep inside. It is this second system that needs to be accessed, befriended, and reconciled.
Just recently at my teaching hospital, a group of psychiatric residents and I interviewed a young woman with temporal lobe epilepsy who was being evaluated following a suicide attempt. The residents asked her standard questions about her symptoms, the medications she was taking, how old she was when the diagnosis was made, what had made her try to kill herself. She responded in a flat, matter-of-fact voice: She’d been five when she was diagnosed. She’d lost her job; she knew she’d been faking it; she felt worthless. For some reason one of the residents asked whether she had been sexually abused. That question surprised me: She had given us no indication that she had had problems with intimacy or sexuality, and I wondered if the doctor was pursuing a private agenda.
Yet the story our patient told did not explain why she had fallen apart after losing her job. So I asked her what it had been like for that five-year-old girl to be told that something was wrong with her brain. That forced her to check in with herself, as she had no ready-made script for that question. In a subdued tone of voice she told us that the worst part of her diagnosis was that afterward her father wanted nothing more to do with her: “He just saw me as a defective child.” Nobody had supported her, she said, so she basically had to manage by herself.
I then asked her how she felt now about that little girl with newly diagnosed epilepsy who was left on her own. Instead of crying for her loneliness or being angry about the lack of support, she said fiercely: “She was stupid, whiny, and dependent. She should have stepped up to the plate and sucked it up.” That passion obviously came from the part of her that had valiantly tried to cope with her distress, and I acknowledged that it probably had helped her survive back then. I asked her to allow that frightened, abandoned girl to tell her what it had been like to be all alone, her illness compounded by family rejection. She started to sob and kept quiet for a long time until finally she said: “No, she did not deserve that. She should have been supported; somebody should have looked after her.” Then she shifted again and proudly told me about her accomplishments—how much she’d achieved despite that lack of support. Public story and inner experience finally met.
THE BODY IS THE BRIDGE
Trauma stories lessen the isolation of trauma, and they provide an explanation for why people suffer the way they do. They allow doctors to make diagnoses, so that they can address problems like insomnia, rage, nightmares, or numbing. Stories can also provide people with a target to blame. Blaming is a universal human trait that helps people feel good while feeling bad, or, as my old teacher Elvin Semrad used to say: “Hate makes the world go round.” But stories also obscure a more important issue, namely, that trauma radically changes people: that in fact they no longer are “themselves.”
It is excruciatingly difficult to put that feeling of no longer being yourself into words. Language evolved primarily to share “things out there,” not to communicate our inner feelings, our interiority. (Again, the language center of the brain is about as far removed from the center for experiencing one’s self as is geographically possible.) Most of us are better at describing someone else than we are at describing ourselves. As I once heard Harvard psychologist Jerome Kagan say: “The task of describing most private experiences can be likened to reaching down to a deep well to pick up small fragile crystal figures while you are wearing thick leather mittens.”11
We can get past the slipperiness of words by engaging the self-observing, body-based self system, which speaks through sensations, tone of voice, and body tensions. Being able to perceive visceral sensations is the very foundation of emotional awareness.12 If a patient tells me that he was eight when his father deserted the family, I am likely to stop and ask him to check in with himself: What happens inside when he tells me about that boy who never saw his father again? Where is it registered in his body? When you activate your gut feelings and listen to your heartbreak—when you follow the interoceptive pathways to your innermost recesses—things begin to change.
WRITING TO YOURSELF
There are other ways to access your inner world of feelings. One of the most effective is through writing. Most of us have poured out our hearts in angry, accusatory, plaintive, or sad letters after people have betrayed or abandoned us. Doing so almost always makes us feel better, even if we never send them. When you write to yourself, you don’t have to worry about other people’s judgment— you just listen to your own thoughts and let their flow take over. Later, when you reread what you wrote, you often discover surprising truths.
As functioning members of society, we’re supposed to be “cool” in our day-to-day interactions and subordinate our feelings to the task at hand. When we talk with someone with whom we don’t feel completely safe, our social editor jumps in on full alert and our guard is up. Writing is different. If you ask your editor to leave you alone for a while, things will come out that you had no idea were there. You are free to go into a sort of a trance state in which your pen (or keyboard) seems to channel whatever bubbles up from inside. You can connect those self-observing and narrative parts of your brain without worrying about the reception you’ll get.
In the practice called free writing, you can use any object as your own personal Rorschach test for entering a stream of associations. Simply write the first thing that comes to your mind as you look at the object in front of you and then keep going without stopping, rereading, or crossing out. A wooden spoon on the counter may trigger memories of making tomato sauce with your grandmother—or of being beaten as a child. The teapot that’s been passed down for generations may take you meandering to the furthest reaches of your mind to the loved ones you’ve lost or family holidays that were a mix of love and conflict. Soon an image will emerge, then a memory, and then a paragraph to record it. Whatever shows up on the paper will be a manifestation of associations that are uniquely yours.
My patients often bring in fragments of writing and drawings about memories that they may not yet be ready to discuss. Reading the content out loud would probably overwhelm them, but they want me to be aware of what they are wrestling with. I tell them how much I appreciate their courage in allowing themselves to explore hitherto hidden parts of themselves and in entrusting me with them. These tentative communications guide my treatment plan—for example, by helping me to decide whether to add somatic processing, neurofeedback, or EMDR to our current work.
As far as I’m aware, the first systematic test of the power of language to relieve trauma was done in 1986, when James Pennebaker at the University of Texas in Austin turned his introductory psychology class into an experimental laboratory. Pennebaker started off with a healthy respect for the importance of inhibition, of keeping things to yourself, which he viewed as the glue of civilization.13 But he also assumed that people pay a price for trying to suppress being aware of the elephant in the room.
He began by asking each student to identify a deeply personal experience that they’d found very stressful or traumatic. He then divided the class into three groups: One would write about what was currently going on in their lives; the second would write about the details of the traumatic or stressful event; and the third would recount the facts of the experience, their feelings and emotions about it, and what impact they thought this event had had on their lives. All of the students wrote continuously for fifteen minutes on four consecutive days while sitting alone in a small cubicle in the psychology building.
The students took the study very seriously; many revealed secrets that they had never told anyone. They often cried as they wrote, and many confided in the course assistants that they’d become preoccupied with these experiences. Of the two hundred participants, sixty-five wrote about a childhood trauma. Although the death of a family member was the most frequent topic, 22 percent of the women and 10 percent of the men reported sexual trauma prior to the age of seventeen.
The researchers asked the students about their health and were surprised how often the students spontaneously reported histories of major and minor health problems: cancer, high blood pressure, ulcers, flu, headaches, and earaches.14 Those who reported a traumatic sexual experience in childhood had been hospitalized an average of 1.7 days in the previous year—almost twice the rate of the others.
The team then compared the number of visits to the student health center participants had made during the month prior to the study to the number in the month following it. The group that had written about both the facts and the emotions related to their trauma clearly benefited the most: They had a 50 percent drop in doctor visits compared with the other two groups. Writing about their deepest thoughts and feelings about traumas had improved their mood and resulted in a more optimistic attitude and better physical health.
When the students themselves were asked to assess the study, they focused on how it had increased their self-understanding: “It helped me think about what I felt during those times. I never realized how it affected me before.” “I had to think and resolve past experiences. One result of the experiment was peace of mind. To have to write about emotions and feelings helped me understand how I felt and why.”15
In a subsequent study Pennebaker asked half of a group of seventy-two students to talk into a tape recorder about the most traumatic experience of their lives; the other half discussed their plans for the rest of the day. As they spoke, researchers monitored their physiological reactions: blood pleasure, heart rate, muscle tension, and hand temperature.16 This study had similar results: Those who allowed themselves to feel their emotions showed significant physiological changes, both immediate and long term. During their confessions blood pressure, heart rate, and other autonomic functions increased, but afterward their arousal fell to levels below where they had been at the start of the study. The drop in blood pressure could still be measured six weeks after the experiment ended.
It is now widely accepted that stressful experiences—whether divorce or final exams or loneliness—have a negative effect on immune function, but this was a highly controversial notion at the time of Pennebaker’s study. Building on his protocols, a team of researchers at the Ohio State University College of Medicine compared two groups of students who wrote either about a personal trauma or about a superficial topic.17 Again, those who wrote about personal traumas had fewer visits to the student health center, and their improved health correlated with improved immune function, as measured by the action of T lymphocytes (natural killer cells) and other immune markers in the blood. This effect was most obvious directly after the experiment, but it could still be the detected six weeks later. Writing experiments from around the world, with grade school students, nursing home residents, medical students, maximum-security prisoners, arthritis sufferers, new mothers, and rape victims, consistently show that writing about upsetting events improves physical and mental health.
Another aspect of Pennebaker’s studies caught my attention: When his subjects talked about intimate or difficult issues, they often changed their tone of voice and speaking style. The differences were so striking that Pennebaker wondered if he had mixed up his tapes. For example, one woman described her plans for the day in a childlike, high-pitched voice, but a few minutes later, when she described stealing one hundred dollars from an open cash register, both the volume and pitch of her voice became so much lower that she sounded like an entirely different person. Alterations in emotional states were also reflected in the subjects’ handwriting. As participants changed topics, they might move from cursive to block letters and back to cursive; there were also variations in the slant of the letters and in the pressure of their pens.
Such changes are called “switching” in clinical practice, and we see them often in individuals with trauma histories. Patients activate distinctly different emotional and physiological states as they move from one topic to another. Switching manifests not only as remarkably different vocal patterns but also in different facial expressions and body movements. Some patients even appear to change their personal identity, from timid to forceful and aggressive or from anxiously compliant to starkly seductive. When they write about their deepest fears, their handwriting often becomes more childlike and primitive.
If patients who present in such dramatically different states are treated as fakes, or if they are told to stop showing their unpredictably annoying parts, they are likely to become mute. They probably will continue to seek help, but after they have been silenced they will transmit their cries for help not by talking but by acting: with suicide attempts, depression, and rage attacks. As we will see in chapter 17, they will improve only if both patient and therapist appreciate the roles that these different states have played in their survival.
ART, MUSIC, AND DANCE
There are thousands of art, music, and dance therapists who do beautiful work with abused children, soldiers suffering from PTSD, incest victims, refugees, and torture survivors, and numerous accounts attest to the effectiveness of expressive therapies.18 However, at this point we know very little about how they work or about the specific aspects of traumatic stress they address, and it would present an enormous logistical and financial challenge to do the research necessary to establish their value scientifically.
The capacity of art, music, and dance to circumvent the speechlessness that comes with terror may be one reason they are used as trauma treatments in cultures around the world. One of the few systematic studies to compare nonverbal artistic expression with writing was done by James Pennebaker and Anne Krantz, a San Francisco dance and movement therapist.19 One-third of a group of sixty-four students was asked to disclose a personal traumatic experience through expressive body movements for at least ten minutes a day for three consecutive days and then to write about it for another ten minutes. A second group danced but did not write about their trauma, and a third group engaged in a routine exercise program. Over the three following months members of all groups reported that they felt happier and healthier. However, only the expressive movement group that also wrote showed objective evidence: better physical health and an improved grade-point average. (The study did not evaluate specific PTSD symptoms.) Pennebaker and Krantz concluded: “The mere expression of the trauma is not sufficient. Health does appear to require translating experiences into language.”
However, we still do not know whether this conclusion—that language is essential to healing—is, in fact, always true. Writing studies that have focused on PTSD symptoms (as opposed to general health) have been disappointing. When I discussed this with Pennebaker, he cautioned me that most writing studies of PTSD patients have been done in group settings where participants were expected to share their stories. He reiterated the point I’ve made above —that the object of writing is to write to yourself, to let your self know what you have been trying to avoid.
THE LIMITS OF LANGUAGE
Trauma overwhelms listeners as well as speakers. In The Great War in Modern Memory, his masterful study of World War I, Paul Fussell comments brilliantly on the zone of silence that trauma creates:
One of the cruxes of war. . . is the collision between events and the language available—or thought appropriate—to describe them. . . . Logically there is no reason why the English language could not perfectly well render the actuality of . . . warfare: it is rich in terms like blood, terror, agony, madness, shit, cruelty, murder, sell-out, pain and hoax, as well as phrases like legs blown off, intestines gushing out over his hands, screaming all night, bleeding to death from the rectum, and the like. . . . The problem was less one of “language” than of gentility and optimism. . . . The real reason [that soldiers fall silent] is that soldiers have discovered that no one is very interested in the bad news they have to report. What listener wants to be torn and shaken when he doesn’t have to be? We have made unspeakable mean indescribable: it really means nasty.20
Talking about painful events doesn’t necessarily establish community— often quite the contrary. Families and organizations may reject members who air the dirty laundry; friends and family can lose patience with people who get stuck in their grief or hurt. This is one reason why trauma victims often withdraw and why their stories become rote narratives, edited into a form least likely to provoke rejection.
It is an enormous challenge to find safe places to express the pain of trauma, which is why survivor groups like Alcoholics Anonymous, Adult Children of Alcoholics, Narcotics Anonymous, and other support groups can be so critical. Finding a responsive community in which to tell your truth makes recovery possible. That is also why survivors need professional therapists who are trained to listen to the agonizing details of their lives. I recall the first time a veteran told me about killing a child in Vietnam. I had a vivid flashback to when I was about seven years old and my father told me that a child next door had been beaten to death by Nazi soldiers in front of our house for showing a lack of respect. My reaction to the veteran’s confession was too much to bear, and I had to end the session. That is why therapists need to have done their own intensive therapy, so they can take care of themselves and remain emotionally available to their patients, even when their patients’ stories arouse feelings of rage or revulsion.
A different problem arises when trauma victims themselves become literally speechless—when the language area of the brain shuts down.21 I have seen this shutdown in the courtroom in many immigration cases and also in a case brought against a perpetrator of mass slaughter in Rwanda. When asked to testify about their experiences, victims often become so overwhelmed that they are barely able to speak or are hijacked into such panic that they can’t clearly articulate what happened to them. Their testimony is often dismissed as being too chaotic, confused, and fragmented to be credible.
Others try to recount their history in a way that keeps them from being triggered. This can make them come across as evasive and unreliable witnesses. I have seen dozens of legal cases dismissed because asylum seekers were unable to give coherent accounts of their reasons for fleeing. I’ve also known numerous veterans whose claims were denied by the Veterans Administration because they could not tell precisely what had happened to them.
Confusion and mutism are routine in therapy offices: We fully expect that our patients will become overwhelmed if we keep pressing them for the details of their story. For that reason we’ve learned to “pendulate” our approach to trauma, to use a term coined by my friend Peter Levine. We don’t avoid confronting the details, but we teach our patients how to safely dip one toe in the water and then take it out again, thus approaching the truth gradually.
We start by establishing inner “islands of safety” within the body.22 This means helping patients identify parts of the body, postures, or movements where they can ground themselves whenever they feel stuck, terrified, or enraged. These parts usually lie outside the reach of the vagus nerve, which carries the messages of panic to the chest, abdomen, and throat, and they can serve as allies in integrating the trauma. I might ask a patient if her hands feel okay, and if she says yes, I’ll ask her to move them, exploring their lightness and warmth and flexibility. Later, if I see her chest tighten and her breath almost disappear, I can stop her and ask her to focus on her hands and move them, so that she can feel herself as separate from the trauma. Or I might ask her to focus on her out breath and notice how she can change it, or ask her to lift her arms up and down with each breath—a qigong movement.
For some patients tapping acupressure points is a good anchor.23 I ask others to feel the weight of their body in the chair or to plant their feet on the floor. I might ask a patient who is collapsing into silence to see what happens when he sits up straight. Some patients discover their own islands of safety—they begin to “get” that they can create body sensations to counterbalance feeling out of control. This sets the stage for trauma resolution: pendulating between states of exploration and safety, between language and body, between remembering the past and feeling alive in the present.
DEALING WITH REALITY
Dealing with traumatic memories is, however, just the beginning of treatment. Numerous studies have found that people with PTSD have more general problems with focused attention and with learning new information.24 Alexander McFarlane did a simple test: He asked a group of people to name as many words beginning with the letter B as they could in one minute. Normal subjects averaged fifteen words; those with PTSD averaged three or four. Normal subjects hesitated when they saw threatening words like “blood,” “wound,” or “rape”; McFarlane’s PTSD subjects reacted just as hesitantly to ordinary words like “wool,” “ice cream,” and “bicycle.”25
After a while most people with PTSD don’t spend a great deal of time or effort on dealing with the past—their problem is simply making it through the day. Even traumatized patients who are making real contributions in teaching, business, medicine, or the arts and who are successfully raising their children expend a lot more energy on the everyday tasks of living than do ordinary mortals.
Yet another pitfall of language is the illusion that our thinking can easily be corrected if it doesn’t “make sense.” The “cognitive” part of cognitive behavioral therapy focuses on changing such “dysfunctional thinking.” This is a top-down approach to change in which the therapist challenges or “reframes” negative cognitions, as in “Let’s compare your feelings that you are to blame for your rape with the actual facts of the matter” or “Let’s compare your terror of driving with the statistics about road safety today.”
I’m reminded of the distraught woman who once came to our clinic asking for help with her two-month-old because the baby was “so selfish.” Would she have benefited from a fact sheet on child development or an explanation of the concept of altruism? Such information would be unlikely to help her until she gained access to the frightened, abandoned parts of herself—the parts expressed by her terror of dependence.
There is no question traumatized people have irrational thoughts: “I was to blame for being so sexy.” “The other guys weren’t afraid—they’re real men.” “I should have known better than to walk down that street.” It’s best to treat those thoughts as cognitive flashbacks—you don’t argue with them any more than you would argue with someone who keeps having visual flashbacks of a terrible accident. They are residues of traumatic incidents: thoughts they were thinking when, or shortly after, the traumas occurred that are reactivated under stressful conditions. A better way to treat them is with EMDR, the subject of the following chapter.
BECOMING SOME BODY
The reason people become overwhelmed by telling their stories, and the reason they have cognitive flashbacks, is that their brains have changed. As Freud and Breuer observed, trauma does not simply act as a releasing agent for symptoms. Rather, “the psychical trauma—or more precisely the memory of the trauma— acts like a foreign body which long after its entry must continue to be regarded as an agent that still is at work.”26 Like a splinter that causes an infection, it is the body’s response to the foreign object that becomes the problem more than the object itself.
Modern neuroscience solidly supports Freud’s notion that many of our conscious thoughts are complex rationalizations for the flood of instincts, reflexes, motives, and deep-seated memories that emanate from the unconscious. As we have seen, trauma interferes with the proper functioning of brain areas that manage and interpret experience. A robust sense of self—one that allows a person to state confidently, “This is what I think and feel” and “This is what is going on with me”—depends on a healthy and dynamic interplay among these areas.
Almost every brain-imaging study of trauma patients finds abnormal activation of the insula. This part of the brain integrates and interprets the input from the internal organs—including our muscles, joints, and balance (proprioceptive) system—to generate the sense of being embodied. The insula can transmit signals to the amygdala that trigger fight/fight responses. This does not require any cognitive input or any conscious recognition that something has gone awry—you just feel on edge and unable to focus or, at worst, have a sense of imminent doom. These powerful feelings are generated deep inside the brain and cannot be eliminated by reason or understanding.
Being constantly assaulted by, but consciously cut off from, the origin of bodily sensations produces alexithymia: not being able to sense and communicate what is going on with you. Only by getting in touch with your body, by connecting viscerally with your self, can you regain a sense of who you are, your priorities and values. Alexithymia, dissociation, and shutdown all involve the brain structures that enable us to focus, know what we feel, and take action to protect ourselves. When these essential structures are subjected to inescapable shock, the result may be confusion and agitation, or it may be emotional detachment, often accompanied by out-of-body experiences—the feeling you’re watching yourself from far away. In other words trauma makes people feel like either some body else, or like no body. In order to overcome trauma, you need help to get back in touch with your body, with your Self.
There is no question that language is essential: Our sense of Self depends on being able to organize our memories into a coherent whole.27 This requires well-functioning connections between the conscious brain and the self system of the body—connections that often are damaged by trauma. The full story can be told only after those structures are repaired and after the groundwork has been laid: after no body becomes some body.
Was it a vision, or a waking dream?
Fled is that music;—Do I wake or sleep?
—John Keats
rage
David, a middle-aged contractor, came to see me because his violent attacks were making his home a living hell. During our first session he told me a story about something that had happened to him the summer he was twenty-three. He was working as a lifeguard, and one afternoon a group of kids were roughhousing in the pool and drinking beer. David told them alcohol was not allowed. In response the boys attacked him, and one of them took out his left eye with a broken beer bottle. Thirty years later he still had nightmares and flashbacks about the stabbing.
He was merciless in his criticisms of his own teenage son and often yelled at him for the slightest infraction, and he simply could not bring himself to show any affection toward his wife. On some level he felt that the tragic loss of his eye gave him permission to abuse other people, but he also hated the angry, vengeful person he had become. He had noticed that his efforts to manage his rage made him chronically tense, and he wondered if his fear of losing control had made love and friendship impossible.
During his second visit I introduced a procedure called eye movement desensitization and reprocessing (EMDR). I asked David to go back to the details of his assault and bring to mind his images of the attack, the sounds he had heard, and the thoughts that had gone through his mind. “Just let those moments come back,” I told him.
I then asked him to follow my index finger as I moved it slowly back and forth about twelve inches from his right eye. Within seconds a cascade of rage and terror came to the surface, accompanied by vivid sensations of pain, blood running down his cheek, and the realization that he couldn’t see. As he reported these sensations, I made an occasional encouraging sound and kept moving my finger back and forth. Every few minutes I stopped and asked him to take a deep breath. Then I asked him to pay attention to what was now on his mind, which was a fight he had had in school. I told him to notice that and to stay with that memory. Other memories emerged, seemingly at random: looking for his assailants everywhere, wanting to hurt them, getting into barroom brawls. Each time he reported a new memory or sensation, I urged him to notice what was coming to mind and resumed the finger movements.
At the end of that visit he looked calmer and visibly relieved. He told me that the memory of the stabbing had lost its intensity—it was now something unpleasant that had happened a long time ago. “It really sucked,” he said thoughtfully, “and it kept me off-kilter for years, but I’m surprised what a good life I eventually was able to carve out for myself.”
Our third session, the following week, dealt with the aftermath of the trauma: how he had used drugs and alcohol for years to cope with his rage. As we repeated the EMDR sequences, still more memories arose. David remembered talking with a prison guard he knew about having his incarcerated assailant killed and then changing his mind. Recalling this decision was profoundly liberating: He had come to see himself as a monster who was barely in control, but realizing that he’d turned away from revenge put him back in touch with a mindful, generous side of himself.
Next he spontaneously realized he was treating his son the way he had felt toward his teenaged attackers. As our session ended, he asked if I could meet with him and his family so he could tell his son what had happened and ask for his forgiveness. At our fifth and final session he reported that he was sleeping better and said that for the first time in his life he felt a sense of inner peace. A year later he called to report not only that his he and wife had grown closer and had started to practice yoga together but also that he laughed more and took real pleasure in his gardening and woodworking.
LEARNING ABOUT EMDR
My experience with David is one of many I have had over the past two decades in which EMDR helped to make painful re-creations of the trauma a thing of the past. My introduction to this method came through Maggie, a spunky young psychologist who ran a halfway house for sexually abused girls. Maggie got into one confrontation after another, clashing with nearly everybody—except the thirteen-and fourteen-year-old girls she cared for. She did drugs, had dangerous and often violent boyfriends, had frequent altercations with her bosses, and moved from place to place because she could not tolerate her roommates (nor they her). I never understood how she had mobilized enough stability and concentration to earn a PhD in psychology from a reputable graduate school.
Maggie had been referred to a therapy group I was running for women with similar problems. During her second meeting she told us that her father had raped her twice, once when she was five years old and once when she was seven. She was convinced it had been her fault. She loved her daddy, she explained, and she must have been so seductive that he could not control himself. Listening to her I thought, “She might not blame her father, but she sure is blaming just about everybody else”—including her previous therapists for not helping her get better. Like many trauma survivors, she told one story with words and another in her actions, in which she kept replaying various aspects of her trauma.
Then one day Maggie came to the group eager to discuss a remarkable experience she’d had the previous weekend at an EMDR training for professionals. At that time I’d heard only that EMDR was a new fad in which therapists wiggled their fingers in front of patients’ eyes. To me and my academic colleagues, it sounded like yet another of the crazes that have always plagued psychiatry, and I was convinced that this would turn out to be another of Maggie’s misadventures.
Maggie told us that during her EMDR session she had vividly remembered her father’s rape when she was seven—remembered it from inside her child’s body. She could feel physically how small she was; she could feel her father’s huge body on top of her and could smell the alcohol on his breath. And yet, she told us, even as she relived the incident she was able to observe it from the point of view of her twenty-nine-year-old self. She burst into tears: “I was such a little girl. How could a huge man do this to a little girl?” She cried for a while and then said: “It’s over now. I now know what happened. It wasn’t my fault. I was a little girl and there was nothing I could do to keep him from molesting me.”
I was astounded. I had been looking for a long time for a way to help people revisit their traumatic past without becoming retraumatized. It seemed that
Maggie had had an experience as lifelike as a flashback and yet had not been hijacked by it. Could EMDR make it safe for people to access the imprints of trauma? Could it then transform them into memories of events that had happened far in the past?
Maggie had a few more EMDR sessions and remained in our group long enough for us to see how she changed. She was much less angry, but she kept that sardonic sense of humor that I enjoyed so much. A few months later she got involved with a very different kind of man than she’d ever been attracted to before. She left the group, announcing that she’d resolved her trauma, and I decided it was time for me to get trained in EMDR.
EMDR: FIRST EXPOSURES
Like many scientific advances, EMDR originated with a chance observation. One day in 1987 psychologist Francine Shapiro was walking through a park, preoccupied with some painful memories, when she noticed that rapid eye movements produced a dramatic relief from her distress. How could a major treatment modality grow from such a brief experience? How is it possible that such a simple process had not been noted before? Initially skeptical about her observation she subjected her method to years of experimentation and research, gradually building it into a standardized procedure that could be taught and tested in controlled studies.1
I arrived for my first EMDR training in need of some trauma processing myself. A few weeks earlier the Jesuit priest who was chair of my department at Massachusetts General Hospital had suddenly shut down the Trauma Clinic, leaving us scrambling for a new site and new funds to treat our patients, train our students, and conduct our research. At around the same time, my friend Frank Putnam, who was doing the long-term study of sexually abused girls that I discussed in chapter 10, was fired from the National Institutes of Health and Rick Kluft, the country’s foremost expert on dissociation, lost his unit at the Institute of the Pennsylvania Hospital. It might have all been a coincidence, but it felt as if my whole world was under attack.
My distress about the Trauma Clinic seemed like a good test for my EMDR trial. While I was following my partner’s fingers with my eyes, a rapid succession of fuzzy childhood scenes came to mind: intense family dinner-table conversations, confrontations with schoolmates during recess, throwing pebbles at a shed window with my older brother—all of them the sort of vivid, floating, “hypnopompic” images we experience when we slumber late on a Sunday morning, then forget the moment we fully awaken.
After about half an hour my fellow trainee and I revisited the scene in which my boss told me that he was closing my clinic. Now I felt resigned: “Okay, it happened, and now it’s time to move on.” I never looked back; the clinic later reconstituted itself and has thrived ever since. Was EMDR the sole reason I was able to let go of my anger and distress? Of course I’ll never know for certain, but my mental journey—through unrelated childhood scenes to putting the episode to rest—was unlike anything I had experienced in talk therapy.
What happened next, when it was my turn to administer EMDR, was even more intriguing. We rotated to a different group, and my new fellow student, whom I’d never met before, told me he wanted to address some painful childhood incidents involving his father, but he did not want to discuss them. I had never worked on anybody’s trauma without knowing “the story,” and I was annoyed and flustered by his refusal to share any details. While I was moving my fingers in front of his eyes, he looked intensely distressed—he began sobbing, and his breathing became rapid and shallow. But each time I asked him the questions that the protocol called for, he refused to tell me what came to his mind.
At the end of our forty-five-minute session, the first thing my colleague said was that he’d found dealing with me so unpleasant that he would never refer a patient to me. Otherwise, he remarked, the EMDR session had resolved the matter of his father’s abuse. While I was skeptical and suspected that his rudeness toward me was a carryover from unresolved feelings toward his father, there was no question that he appeared much more relaxed.
I turned to my EMDR trainer, Gerald Puk, and told him how flummoxed I was. This man clearly did not like me, and had looked profoundly distressed during the EMDR session, but now he was telling me that his long-standing misery was gone. How could I possibly know what he had or had not resolved if he was unwilling to tell me what had happened during the session?
Gerry smiled and asked if by chance I had become a mental health professional in order to solve some of my own personal issues. I confirmed that most people who knew me thought that might be the case. Then he asked if I found it meaningful when people told me their trauma stories. Again, I had to agree with him. Then he said: “You know, Bessel, maybe you need to learn to put your voyeuristic tendencies on hold. If it’s important for you to hear trauma
stories, why don’t you go to a bar, put a couple of dollars on the table, and say to your neighbor, ‘I’ll buy you a drink if you tell me your trauma story.’ But you really need to know the difference between your desire to hear stories and your patient’s internal process of healing.” I took Gerry’s admonition to heart and ever since have enjoyed repeating it to my students.
I left my EMDR training preoccupied with three issues that fascinate me to this day:
EMDR loosens up something in the mind/brain that gives people rapid access to loosely associated memories and images from their past. This seems to help them put the traumatic experience into a larger context or perspective.
People may be able to heal from trauma without talking about it. EMDR enables them to observe their experiences in a new way, without verbal give-and-take with another person.
EMDR can help even if the patient and the therapist do not have a trusting relationship. This was particularly intriguing because trauma, understandably, rarely leaves people with an open, trusting heart.
In the years since, I have done EMDR with patients who spoke Swahili, Mandarin, and Breton, all languages in which I can say only, “Notice that,” the key EMDR instruction. (I always had a translator available, but primarily to explain the steps of the process.) Because EMDR doesn’t require patients to speak about the intolerable or explain to a therapist why they feel so upset, it allows them to stay fully focused on their internal experience, with sometimes extraordinary results.
STUDYING EMDR
The Trauma Clinic was saved by a manager at the Massachusetts Department of Mental Health who had followed our work with children and now asked us to take on the task of organizing the community trauma response team for the Boston area. That was enough to cover our basic operations, and the rest was supplied by an energetic staff who loved what we were doing—including the newly discovered power of EMDR to cure some of the patients whom we’d been unable to help before.
My colleagues and I began to show one another videotapes of our EMDR sessions with PTSD patients, which enabled us to observe dramatic week-by-week improvements. We then started to formally measure their progress on a standard PTSD rating scale. We also arranged with Elizabeth Matthew, a young neuroimaging specialist at the New England Deaconess Hospital, to have twelve patients’ brains scanned before and after their treatment. After only three EMDR sessions eight of the twelve had shown a significant decrease in their PTSD scores. On their scans we could see a sharp increase in prefrontal lobe activation after treatment, as well as much more activity in the anterior cingulate and the basal ganglia. This shift could account for the difference in how they now experienced their trauma.
One man reported: “I remember it as though it was a real memory, but it was more distant. Typically, I drowned in it, but this time I was floating on top. I had the feeling that I was in control.” A woman told us: “Before, I felt each and every step of it. Now it is like a whole, instead of fragments, so it is more manageable.” The trauma had lost its immediacy and become a story about something that happened a long time ago.
We subsequently secured funding from the National Institutes of Mental Health to compare the effects of EMDR with standard doses of Prozac or a placebo.2 Of our eighty-eight subjects thirty received EMDR, twenty-eight Prozac, and the rest the sugar pill. As often happens, the people on placebo did well. After eight weeks their 42 percent improvement was greater than that for many other treatments that are promoted as “evidence based.”
The group on Prozac did slightly better than the placebo group, but barely so. This is typical of most studies of drugs for PTSD: Simply showing up brings about a 30 percent to 42 percent improvement; when drugs work, they add an additional 5 percent to 15 percent. However, the patients on EMDR did substantially better than those on either Prozac or the placebo: After eight EMDR sessions one in four were completely cured (their PTSD scores had dropped to negligible levels), compared with one in ten of the Prozac group. But the real difference occurred over time: When we interviewed our subjects eight months later, 60 percent of those who had received EMDR scored as being completely cured. As the great psychiatrist Milton Erickson said, once you kick the log, the river will start flowing. Once people started to integrate their traumatic memories, they spontaneously continued to improve. In contrast, all those who had taken Prozac relapsed when they went off the drug.
This study was significant because it demonstrated that a focused, trauma-specific therapy for PTSD like EMDR could be much more effective than medication. Other studies have confirmed that if patients take Prozac or related drugs like Celexa, Paxil, and Zoloft, their PTSD symptoms often improve, but only as long as they keep taking them. This makes drug treatment much more expensive in the long run. (Interestingly, despite Prozac’s status as a major antidepressant, in our study EMDR also produced a greater reduction in depression scores than taking the antidepressant.)
Another key finding of our study: Adults with histories of childhood trauma responded very differently to EMDR from those who were traumatized as adults. At the end of eight weeks, almost half of the adult-onset group that received EMDR scored as completely cured, while only 9 percent of the child-abuse group showed such pronounced improvement. Eight months later the cure rate was 73 percent for the adult-onset group, compared with 25 percent for those with histories of child abuse. The child-abuse group had small but consistently positive responses to Prozac.
These results reinforce the findings that I reported in chapter 9: Chronic childhood abuse causes very different mental and biological adaptations than discrete traumatic events in adulthood. EMDR is a powerful treatment for stuck traumatic memories, but it doesn’t necessarily resolve the effects of the betrayal and abandonment that accompany physical or sexual abuse in childhood. Eight weeks of therapy of any kind is rarely sufficient to resolve the legacy of longstanding trauma.
As of 2014 our EMDR study had the most positive outcome of any published study of people who developed their PTSD in reaction to a traumatic event as an adult. But despite these results, and those of dozens of other studies, many of my colleagues continue to be skeptical about EMDR—perhaps because it seems too good to be true, too simple to be so powerful. I surely can understand that sort of skepticism—EMDR is an unusual procedure. Interestingly, in the first solid scientific study using EMDR in combat veterans with PTSD, EMDR was expected to do so poorly that it was included as the control condition for comparison with biofeedback-assisted relaxation therapy. To the researchers’ surprise, twelve sessions of EMDR turned out to be the more effective treatment.3 EMDR has since become one of the treatments for PTSD sanctioned by the Department of Veterans Affairs.
IS EMDR A FORM OF EXPOSURE THERAPY?
Some psychologists have hypothesized that EMDR actually desensitizes people to the traumatic material and thus is related to exposure therapy. A more accurate description would be that it integrates the traumatic material. As our research showed, after EMDR people thought of the trauma as a coherent event in the past, instead of experiencing sensations and images divorced from any context.
Memories evolve and change. Immediately after a memory is laid down, it undergoes a lengthy process of integration and reinterpretation—a process that automatically happens in the mind/brain without any input from the conscious self. When the process is complete, the experience is integrated with other life events and stops having a life of its own.4 As we have seen, in PTSD this process fails and the memory remains stuck—undigested and raw.
Unfortunately, few psychologists are taught during their training how the memory-processing system in the brain works. This omission can lead to misguided approaches to treatment. In contrast to phobias (such as a spider phobia, which is based on a specific irrational fear), posttraumatic stress is the result of a fundamental reorganization of the central nervous system based on having experienced an actual threat of annihilation, (or seeing someone else being annihilated), which reorganizes self experience (as helpless) and the interpretation of reality (the entire world is a dangerous place).
During exposure patients initially become extremely upset. As they revisit the traumatic experience, they show sharp increases in their heart rate, blood pressure, and stress hormones. But if they manage to stay with the treatment and keep reliving their trauma, they slowly become less reactive and less prone to disintegrate when they recall the event. As a result, they get lower scores on their PTSD ratings. However, as far as we know, simply exposing someone to the old trauma does not integrate the memory into the overall context of their lives, and it rarely restores them to the level of joyful engagement with people and pursuits they had prior to the trauma.
In contrast, EMDR, as well as the treatments discussed in subsequent chapters—internal family systems, yoga, neurofeedback, psychomotor therapy, and theater—focus not only on regulating the intense memories activated by trauma but also on restoring a sense of agency, engagement, and commitment through ownership of body and mind.
PROCESSING TRAUMA WITH EMDR
Kathy was a twenty-one-year-old student at a local university. When I first met her, she looked terrified. She had been in psychotherapy for three years with a therapist whom she trusted and felt understood by but with whom she was not making any progress. After her third suicide attempt her university health service referred her to me, hoping that the new technique I’d told them about could help her.
Like several of my other traumatized patients, Kathy was able to become completely absorbed in her studies: When she read a book or wrote a research paper, she could block out everything else about her life. This enabled her to be a competent student, even when she had no idea how to establish a loving relationship with herself, let alone with an intimate partner.
Kathy told me that her father had used her for many years for child prostitution, which would normally have made me think of using EMDR only as an adjunctive therapy. However, she turned out to be an EMDR virtuoso and recovered completely after eight sessions, the shortest time thus far in my experience for someone with a history of severe childhood abuse. Those sessions took place fifteen years ago, and I recently met with her to discuss the pros and cons of her adopting a third child. She was a delight: smart, funny, and joyfully engaged with her family and her work as an assistant professor of child development.
I’d like to share my notes on Kathy’s fourth EMDR treatment, not only to demonstrate what typically happens in such a session but also to reveal the human mind in action as it integrates a traumatic experience. No brain scan, blood test, or rating scale can measure this, and even a video recording can convey only a shadow of how EMDR can unleash the imaginative powers of the mind.
Kathy sat with her chair at a forty-five-degree angle to mine, so that we were about four feet apart. I asked her to bring a particularly painful memory to mind and encouraged her to recall what she had heard, saw, thought, and felt in her body as it took place. (My records do not show whether she told me what the particular memory was; my guess is probably not, since I did not write it down.)
I asked her whether she was now “in the memory,” and when she said yes, I asked her how real it felt on a scale of one to ten. About a nine, she said. Then I asked her to follow my moving finger with her eyes. From time to time, after completing a set of about twenty-five eye movements, I might say: “Take a deep breath,” followed by: “What do you get now?” or “What comes to mind now?” Kathy would then tell me what she was thinking. Whenever her tone of voice,
facial expression, body movements, or breathing patterns indicated that this was an emotionally significant theme, I would say, “Notice that,” and start another set of eye movements, during which she did not speak. Other than uttering those few words, I remained silent for the next forty-five minutes.
Here is the association Kathy reported after the first eye-movement sequence: “I realize that I have scars—from when he tied my hands behind my back. The other scar is when he marked me to claim me as his, and there [she points] are bite marks.” She looked stunned but surprisingly calm as she recalled, “I remember being doused in gasoline—he took Polaroid pictures of me —and then I was submerged in water. I was gang raped by my father and two of his friends; I was tied to a table; I remember them raping me with Budweiser bottles.”
My stomach was clenching, but I didn’t comment beyond asking Kathy to keep those memories in mind. After about thirty more back-and-forth movements I stopped when I saw that she was smiling. When I asked what she was thinking, she said, “I was in a karate class; it was great! I really kicked butt! I saw them backing off. I yelled, ‘Don’t you see you are hurting me? I am not your girlfriend.’” I said, “Stay there,” and began the next sequence. When it ended, Kathy said: “I have an image of two me’s—this smart, pretty little girl... and that little slut. All these women who could not take care of themselves or me or their men—leaving it up to me to service all these men.” She started to sob during the next sequence, and when we stopped, she said: “I saw how little I was —the brutalization of the little girl. It was not my fault.” I nodded and said, “That’s right—stay there.” The next round ended with Kathy reporting: “I’m picturing my life now—my big me holding my little me—saying, ‘You are safe now.’” I nodded encouragingly and continued.
The images kept coming: “I have pictures of a bulldozer flattening the house I grew up in. It’s over!” Then Kathy started on a different track: “I am thinking about how much I like Jeffrey [a boy in one of her classes]. Thinking that he might not want to hang out with me. Thinking I can’t handle it. I have never been someone’s girlfriend before and I don’t know how.” I asked her what she thought she needed to know and began the next sequence. “Now, there is a person who just wants to be with me—it is too simple. I don’t know how to just be myself around men. I am petrified.”
As she tracked my finger, Kathy started to sob. When I stopped, she told me: “I had an image of Jeffrey and me sitting in the coffeehouse. My father comes in the door. He starts screaming at the top of his lungs and he is wielding
an ax; he says, ‘I told you that you belong to me.’ He puts me on top of the table —then he rapes me, and then he rapes Jeffrey.” She was crying hard now. “How can you be open with somebody when you have visions of your dad raping you and then raping us both?” I wanted to comfort her, but I knew it was more important to keep her associations moving. I asked her to focus on what she felt in her body: “I feel it in my forearms, in my shoulders, and my right chest. I just want to be held.” We continued the EMDR and when we stopped, Kathy looked relaxed. “I heard Jeffrey say it’s okay, that he was sent here to take care of me. And that it was not anything that I did and that he just wants to be with me for my sake.” Again I asked what she felt in her body. “I feel really peaceful. A little bit shaky—like when you’re using new muscles. Some relief. Jeffrey knows all this already. I feel like I’m alive and that it is all over. But I am afraid that my father has another little girl, and that makes me very, very sad. I want to save her.”
But as we continued the trauma returned, together with other thoughts and images: “I need to throw up. . . . I have intrusions of lots of smells—bad cologne, alcohol, vomit.” A few minutes later Kathy was crying profusely: “I really feel my mom here now. It feels like she wants me to forgive her. I have the sense that the same thing happened to her—she is apologizing to me over and over. She’s telling me that this happened to her—that it was my grandfather. She’s also telling me that my grandmother is really sorry for not being there to protect me.” I kept asking her to take deep breaths and stay with whatever was coming up.
At the end of the next sequence Kathy said: “I feel like it’s over. I felt my grandmother holding me at my current age—telling me that she is so sorry she married my grandfather. That she and my mom are making sure that it stops here.” After one final EMDR sequence Kathy was smiling: “I have an image of pushing my father out of the coffeehouse and Jeffrey locking the door behind him. He stands outside. You can see him through the glass—everybody’s making fun of him.”
With the help of EMDR Kathy was able to integrate the memories of her trauma and call on her imagination to help her lay them to rest, arriving at a sense of completion and control. She did so with minimal input from me and without any discussion of the particulars of her experiences. (I never felt a reason to question their accuracy; her experiences were real to her, and my job was to help her deal with them in the present.) The process freed something in her mind/brain to activate new images, feelings, and thoughts; it was as if her life force emerged to create new possibilities for her future.5
As we’ve seen, traumatic memories persist as split-off, unmodified images, sensations, and feelings. To my mind the most remarkable feature of EMDR is its apparent capacity to activate a series of unsought and seemingly unrelated sensations, emotions, images, and thoughts in conjunction with the original memory. This way of reassembling old information into new packages may be just the way we integrate ordinary, nontraumatic day-to-day experiences.
EXPLORING THE SLEEP CONNECTION
Shortly after learning about EMDR I was asked to speak about my work at the sleep laboratory headed by Allan Hobson at the Massachusetts Mental Health Center. Hobson (together with his teacher, Michel Jouvet)6 was famous for discovering where dreams are generated in the brain, and one of his research assistants, Robert Stickgold, was just then beginning to explore the function of dreams. I showed the group a videotape of a patient who had suffered from severe PTSD for thirteen years after a terrible car accident and who, in only two sessions of EMDR, had transformed from a helpless panicked victim into a confident, assertive woman. Bob was fascinated.
A few weeks later a friend of Stickgold’s family became so depressed after the death of her cat that she had to be hospitalized. The attending psychiatrist concluded that the cat’s death had triggered unresolved memories of the death of the woman’s mother when she was twelve, and he connected her with Roger Solomon, a well-known EMDR trainer, who treated her successfully. Afterward she called Stickgold and said, “Bob, you have to study this. It’s really strange—it has to do with your brain, not your mind.”
Soon afterward an article appeared in the journal Dreaming suggesting that EMDR was related to rapid eye movement (REM) sleep—the phase of sleep in which dreaming occurs.7 Research had already shown that sleep, and dream sleep in particular, plays a major role in mood regulation. As the article in Dreaming pointed out, the eyes move rapidly back and forth in REM sleep, just as they do in EMDR. Increasing our time in REM sleep reduces depression, while the less REM sleep we get, the more likely we are to become depressed.8
Of course, PTSD is notoriously associated with disturbed sleep, and self-medication with alcohol or drugs further disrupts REM sleep. During my time at the VA my colleagues and I had found that the veterans with PTSD frequently woke themselves up soon after going into REM sleep9—probably because they
had activated a trauma fragment during a dream.10 Other researchers have also noticed this phenomenon, but thought that it was irrelevant to understanding PTSD.11
Today we know that both deep sleep and REM sleep play important roles in how memories change over time. The sleeping brain reshapes memory by increasing the imprint of emotionally relevant information while helping irrelevant material fade away.12 In a series of elegant studies Stickgold and his colleagues showed that the sleeping brain can even make sense out of information whose relevance is unclear while we are awake and integrate it into the larger memory system.13
Dreams keep replaying, recombining, and reintegrating pieces of old memories for months and even years.14 They constantly update the subterranean realities that determine what our waking minds pay attention to. And perhaps most relevant to EMDR, in REM sleep we activate more distant associations than in either non-REM sleep or the normal waking state. For example, when subjects are wakened from non-REM sleep and given a word-association test, they give standard responses: hot/cold, hard/soft, etc. Wakened from REM sleep, they make less conventional connections, such as thief/wrong.15 They also solve simple anagrams more easily after REM sleep. This shift toward activation of distant associations could explain why dreams are so bizarre.16
Stickgold, Hobson, and their colleagues thus discovered that dreams help to forge new relationships between apparently unrelated memories.17 Seeing novel connections is the cardinal feature of creativity; as we’ve seen, it’s also essential to healing. The inability to recombine experiences is also one of the striking features of PTSD. While Noam in chapter 4 could imagine a trampoline to save future victims of terrorism, traumatized people are trapped in frozen associations: Anybody who wears a turban will try to kill me; any man who finds me attractive wants to rape me.
Finally, Stickgold suggests a clear link between EMDR and memory processing in dreams: “If the bilateral stimulation of EMDR can alter brain states in a manner similar to that seen during REM sleep then there is now good evidence that EMDR should be able to take advantage of sleep-dependent processes, which may be blocked or ineffective in PTSD sufferers, to allow effective memory processing and trauma resolution.”18 The basic EMDR instruction, “Hold that image in your mind and just watch my fingers moving back and forth,” may very well reproduce what happens in the dreaming brain.
As this book is going to press Ruth Lanius and I are studying how the brain reacts, both while remembering a traumatic event and an ordinary experience, to saccadic eye movements as subjects lie in an fMRI scanner. Stay tuned.
ASSOCIATION AND INTEGRATION
Unlike conventional exposure treatment, EMDR spends very little time revisiting the original trauma. The trauma itself is certainly the starting point, but the focus is on stimulating and opening up the associative process. As our Prozac/EMDR study showed, drugs can blunt the images and sensations of terror, but they remain embedded in the mind and body. In contrast with the subjects who improved on Prozac—whose memories were merely blunted, not integrated as an event that happened in the past, and still caused considerable anxiety—those who received EMDR no longer experienced the distinct imprints of the trauma: It had become a story of a terrible event that had happened a long time ago. As one of my patients said, making a dismissive hand gesture: “It’s over.”
While we don’t yet know precisely how EMDR works, the same is true of Prozac. Prozac has an effect on serotonin, but whether its levels go up or down, and in which brain cells, and why that makes people feel less afraid, is still unclear. We likewise don’t know precisely why talking to a trusted friend gives such profound relief, and I am surprised how few people seem eager to explore that question.19
Clinicians have only one obligation: to do whatever they can to help their patients get better. Because of this, clinical practice has always been a hotbed for experimentation. Some experiments fail, some succeed, and some, like EMDR, dialectical behavior therapy, and internal family systems therapy, go on to change the way therapy is practiced. Validating all these treatments takes decades and is hampered by the fact that research support generally goes to methods that have already been proven to work. I am much comforted by considering the history of penicillin: Almost four decades passed between the discovery of its antibiotic properties by Alexander Fleming in 1928 and the final elucidation of its mechanisms in 1965.
CHAPTER 16 LEARNING TO INHABIT YOUR BODY: YOGA
As we begin to re-experience a visceral reconnection with the needs of our bodies, there is a brand new capacity to warmly love the self. We experience a new quality of authenticity in our caring, which redirects our attention to our health, our diets, our energy, our time management. This enhanced care for the self arises spontaneously and naturally, not as a response to a “should.” We are able to experience an immediate and intrinsic pleasure in self-care.
—Stephen Cope, Yoga and the Quest for the True Self
waiting
T he first time I saw Annie she was slumped over in a chair in my
room wearing faded jeans and a purple Jimmy Cliff T-shirt Her legs w
, . ere
visibly shaking, and she kept staring at the floor even after I invited her in. I had very little information about her, other than that she was forty-seven years old and taught special-needs children. Her body communicated clearly that she was too terrified to engage in conversation—or even to provide routine information about her address or insurance plan. People who are this scared can’t think straight, and any demand to perform will only make them shut down further. If you insist, they’ll run away and you’ll never see them again.
Annie shuffled into my office and remained standing, barely breathing, looking like a frozen bird. I knew we couldn’t do anything until I could help her quiet down. Moving to within six feet of her and making sure she had unobstructed access to the door, I encouraged her to take slightly deeper breaths.
I breathed with her and asked her to follow my example, gently raising my arms from my sides as she inhaled and lowering them as I exhaled, a qigong technique that one of my Chinese students had taught me. She stealthily followed my movements, her eyes still fixed on the floor. We spent about half an hour this way. From time to time I quietly asked her to notice how her feet felt against the floor and how her chest expanded and contracted with each breath. Her breath gradually became slower and deeper, her face softened, her spine straightened a bit, and her eyes lifted to about the level of my Adam’s apple. I began to sense the person behind that overwhelming terror. Finally she looked more relaxed and showed me the glimmer of a smile, a recognition that we both were in the room. I suggested that we stop there for now—I’d made enough demands on her—and asked whether she would like to come back a week later. She nodded and muttered, “You sure are weird.”
As I got to know Annie, I inferred from the notes she wrote and the drawings she gave me that she had been dreadfully abused by both her father and her mother as a very young child. The full story was only gradually revealed, as she slowly learned to call up some of the things that had happened to her without her body being hijacked into uncontrollable anxiety.
I learned that Annie was extraordinarily skilled and caring in her work with special-needs kids. (I tried out quite a few of the techniques she told me about with the children in our own clinic and found them extremely helpful). She would talk freely about the children she taught but would clam up immediately if we verged on her relationships with adults. I knew she was married, but she barely mentioned her husband. She often coped with disagreements and confrontations by making her mind disappear. When she felt overwhelmed she’d cut her arms and breasts with a razor blade. She had spent years in various forms of therapy and had tried many different medications, which had done little to help her deal with the imprints of her horrendous past. She had also been admitted to several psychiatric hospitals to manage her self-destructive behaviors, again without much apparent benefit.
In our early therapy sessions, because Annie could only hint at what she was feeling and thinking before she would shut down and freeze, we focused on calming the physiological chaos within. We used every technique that I had learned over the years, like breathing with a focus on the out breath, which activates the relaxing parasympathetic nervous system. I also taught her to use her fingers to tap a sequence of acupressure points on various parts of her body, a practice often taught under the name EFT (Emotional Freedom Technique),
which has been shown to help patients stay within the window of tolerance and often has positive effects on PTSD symptoms.1
THE LEGACY OF INESCAPABLE SHOCK
Because we can now identify the brain circuits involved in the alarm system, we know, more or less, what was happening in Annie’s brain as she sat that first day in my waiting room: Her smoke detector, her amygdala, had been rewired to interpret certain situations as harbingers of life-threatening danger, and it was sending urgent signals to her survival brain to fight, freeze, or flee. Annie had all these reactions simultaneously—she was visibly agitated and mentally shut down.
As we’ve seen, broken alarm systems can manifest in various ways, and if your smoke detector malfunctions, you cannot trust the accuracy of your perceptions. For example, when Annie started to like me she began to look forward to our meetings, but she would arrive at my office in an intense panic. One day she had a flashback of feeling excited that her father was coming home soon—but later that evening he molested her. For the first time, she realized that her mind automatically associated excitement about seeing someone she loved with the terror of being molested.
Small children are particularly adept at compartmentalizing experience, so that Annie’s natural love for her father and her dread of his assaults were held in separate states of consciousness. As an adult Annie blamed herself for her abuse, because she believed that the loving, excited little girl she once was had led her father on—that she had brought the molestation upon herself. Her rational mind told her this was nonsense, but this belief emanated from deep within her emotional, survival brain, from the basic wiring of her limbic system. It would not change until she felt safe enough within her body to mindfully go back into that experience and truly know how that little girl had felt and acted during the abuse.
THE NUMBING WITHIN
One of the ways the memory of helplessness is stored is as muscle tension or feelings of disintegration in the affected body areas: head, back, and limbs in accident victims, vagina and rectum in victims of sexual abuse. The lives of many trauma survivors come to revolve around bracing against and neutralizing unwanted sensory experiences, and most people I see in my practice have become experts in such self-numbing. They may become serially obese or anorexic or addicted to exercise or work. At least half of all traumatized people try to dull their intolerable inner world with drugs or alcohol. The flip side of numbing is sensation seeking. Many people cut themselves to make the numbing go away, while others try bungee jumping or high-risk activities like prostitution and gambling. Any of these methods can give them a false and paradoxical feeling of control.
When people are chronically angry or scared, constant muscle tension ultimately leads to spasms, back pain, migraine headaches, fibromyalgia, and other forms of chronic pain. They may visit multiple specialists, undergo extensive diagnostic tests, and be prescribed multiple medications, some of which may provide temporary relief but all of which fail to address the underlying issues. Their diagnosis will come to define their reality without ever being identified as a symptom of their attempt to cope with trauma.
The first two years of my therapy with Annie focused on helping her learn to tolerate her physical sensations for what they were—just sensations in the present, with a beginning, a middle, and an end. We worked on helping her stay calm enough to notice what she felt without judgment, so she could observe these unbidden images and feelings as residues of a terrible past and not as unending threats to her life today.
Patients like Annie continuously challenge us to find new ways of helping people regulate their arousal and control their own physiology. That is how my Trauma Center colleagues and I stumbled upon yoga.
FINDING OUR WAY TO YOGA: BOTTOM-UP REGULATION
Our involvement with yoga started in 1998 when Jim Hopper and I first heard about a new biological marker, heart rate variability (HRV), that had recently been discovered to be a good measure of how well the autonomic nervous system is working. As you’ll recall from chapter 5, the autonomic nervous system is our brain’s most elementary survival system, its two branches regulating arousal throughout the body. Roughly speaking, the sympathetic nervous system (SNS) uses chemicals like adrenaline to fuel the body and brain to take action, while the parasympathetic nervous system (PNS) uses acetylcholine to help regulate basic body functions like digestion, wound healing, and sleep and dream cycles. When we’re at our best, these two systems work closely together to keep us in an optimal state of engagement with our environment and with ourselves.
Heart rate variability measures the relative balance between the sympathetic and the parasympathetic systems. When we inhale, we stimulate the SNS, which results in an increase in heart rate. Exhalations stimulate the PNS, which decreases how fast the heart beats. In healthy individuals inhalations and exhalations produce steady, rhythmical fluctuations in heart rate: Good heart rate variability is a measure of basic well-being.
Why is HRV important? When our autonomic nervous system is well balanced, we have a reasonable degree of control over our response to minor frustrations and disappointments, enabling us to calmly assess what is going on when we feel insulted or left out. Effective arousal modulation gives us control over our impulses and emotions: As long as we manage to stay calm, we can choose how we want to respond. Individuals with poorly modulated autonomic nervous systems are easily thrown off balance, both mentally and physically. Since the autonomic nervous system organizes arousal in both body and brain, poor HRV—that is, a lack of fluctuation in heart rate in response to breathing— not only has negative effects on thinking and feeling but also on how the body responds to stress. Lack of coherence between breathing and heart rate makes people vulnerable to a variety of physical illnesses, such as heart disease and cancer, in addition to mental problems such as depression and PTSD.2
In order to study this issue further, we acquired a machine to measure HRV and started to put bands around the chests of research subjects with and without PTSD to record the depth and rhythm of their breathing while little monitors attached to their earlobes picked up their pulse. After we’d tested about sixty subjects, it became clear that people with PTSD have unusually low HRV. In other words, in PTSD the sympathetic and parasympathetic nervous systems are out of sync.3 This added a new twist to the complicated trauma story: We confirmed that yet another brain regulatory system was not functioning as it should.4 Failure to keep this system in balance is one explanation why traumatized people like Annie are so vulnerable to overrespond to relatively minor stresses: The biological systems that are meant to help us cope with the vagaries of life fail to meet the challenge.
Our next scientific question was: Is there a way for people to improve their HRV? I had a personal incentive to explore this question, as I had discovered that my own HRV was not nearly robust enough to guarantee long-term physical health. An Internet search turned up studies showing that marathon running markedly increased HRV. Sadly, that was of little use, since neither I nor our patients were good candidates for the Boston Marathon. Google also listed seventeen thousand yoga sites claiming that that yoga improved HRV, but we were unable to find any supporting studies. Yogis may have developed a wonderful method to help people find internal balance and health, but back in 1998 not much work had been done on evaluating their claims with the tools of the Western medical tradition.
Heart rate variability (HRV) in a well-regulated person. The rising and falling black lines represent breathing, in this case slow and regular inhalations and exhalations. The gray area shows fluctuations in heart rate. Whenever this individual inhales, his heart rate goes up; during exhalations the heart slows down. This pattern of heart rate variability reflects excellent physiological health.
Responding to upset. When someone remembers an upsetting experience, breathing speeds up and becomes irregular, as does heart rate. Heart and breath no longer stay perfectly in sync. This is a normal response.
HRV in PTSD. Breathing is rapid and shallow. Heart rate is slow and out of synch with the breath. This is a typical pattern of a shut-down person with chronic PTSD.
A person with chronic PTSD reliving a trauma memory. Breathing initially is labored and deep, typical of a panic reaction. The heart races out of synch with the breath. This is followed by rapid, shallow breathing and slow heart rate, signs that the person is shutting down.
Since then, however, scientific methods have confirmed that changing the way one breathes can improve problems with anger, depression, and anxiety5 and that yoga can positively affect such wide-ranging medical problems as high blood pressure, elevated stress hormone secretion,6 asthma, and low-back pain.7 However, no psychiatric journal had published a scientific study of yoga for PTSD until our own work appeared in 2014.8
As it happened, a few days after our Internet search a lanky yoga teacher named David Emerson walked through the front door of the Trauma Center. He told us that he’d developed a modified form of hatha yoga to deal with PTSD and that he’d been holding classes for veterans at a local vet center and for women in the Boston Area Rape Crisis Center. Would we be interested in working with him? Dave’s visit eventually grew into a very active yoga program, and in due course we received the first grant from the National Institutes of Health to study the effects of yoga on PTSD. Dave’s work also contributed to my developing my own regular yoga practice and becoming a frequent teacher at Kripalu, a yoga center in the Berkshire Mountains in western Massachusetts. (Along the way, my own HRV pattern improved as well.)
In choosing to explore yoga to improve HRV we were taking an expansive approach to the problem. We could simply have used any of a number of reasonably priced handheld devices that train people to slow their breathing and synchronize it with their heart rate, resulting in a state of “cardiac coherence” like the pattern shown in the first illustration above.9 Today there are a variety of apps that can help improve HRV with the aid of a smartphone.10 In our clinic we have workstations where patients can train their HRV, and I urge all my patients who, for one reason or another, cannot practice yoga, martial arts, or qigong to train themselves at home. (See Resources for more information.)
EXPLORING YOGA
Our decision to study yoga led us deeper into trauma’s impact on the body. Our first experimental yoga classes met in a room generously donated by a nearby studio. David Emerson and his colleagues Dana Moore and Jodi Carey volunteered as instructors, and my research team figured out how we could best measure yoga’s effects on psychological functioning. We put flyers in neighborhood supermarkets and laundromats to advertise our classes and interviewed dozens of people who called in response. Ultimately we selected thirty-seven women who had severe trauma histories and who had already received many years of therapy without much benefit. Half the volunteers were selected at random for the yoga group, while the others would receive a well-established mental health treatment, dialectical behavior therapy (DBT), which teaches people how to apply mindfulness to stay calm and in control. Finally, we commissioned an engineer at MIT to build us a complicated computer that could measure HRV simultaneously in eight different people. (In each study group there were multiple classes, each with no more than eight participants.) While yoga significantly improved arousal problems in PTSD and dramatically improved our subjects’ relationships to their bodies (“I now take care of my body”; “I listen to what my body needs”), eight weeks of DBT did not affect their arousal levels or PTSD symptoms. Thus, our interest in yoga gradually evolved from a focus on learning whether yoga can change HRV (which it can)11 to helping traumatized people learn to comfortably inhabit their tortured bodies.
Over time we also started a yoga program for marines at Camp Lejeune and have worked successfully with various other programs to implement yoga programs for veterans with PTSD. Even though we have no formal research data on the veterans, it looks as if yoga is at least as effective for them as it has been for the women in our studies.
All yoga programs consist of a combination of breath practices (pranayama), stretches or postures (asanas), and meditation. Different schools of yoga emphasize variations in intensity and focus within these core components. For example, variations in the speed and depth of breathing and use of the mouth, nostrils, and throat all produce different results, and some techniques have powerful effects on energy.12 In our classes we keep the approach simple. Many of our patients are barely aware of their breath, so learning to focus on the in and out breath, to notice whether the breath was fast or slow, and to count breaths in some poses can be a significant accomplishment.13
We gradually introduce a limited number of classic postures. The emphasis is not on getting the poses “right” but on helping the participants notice which muscles are active at different times. The sequences are designed to create a rhythm between tension and relaxation—something we hope they will begin to perceive in their day-to-day lives.
We do not teach meditation as such, but we do foster mindfulness by encouraging students to observe what is happening in different parts of the body from pose to pose. In our studies we keep seeing how difficult it is for traumatized people to feel completely relaxed and physically safe in their bodies. We measure our subjects’ HRV by placing tiny monitors on their arms during shavasana, the pose at the end of most classes during which practitioners lie face up, palms up, arms and legs relaxed. Instead of relaxation we picked up too much muscle activity to get a clear signal. Rather than going into a state of quiet repose, our students’ muscles often continue to prepare them to fight unseen enemies. A major challenge in recovering from trauma remains being able to achieve a state of total relaxation and safe surrender.
LEARNING SELF-REGULATION
After seeing the success of our pilot studies, we established a therapeutic yoga program at the Trauma Center. I thought that this might be an opportunity for Annie to develop a more caring relationship with her body, and I urged her to try it. The first class was difficult. Merely being given an adjustment by the instructor was so terrifying that she went home and slashed herself—her malfunctioning alarm system interpreted even a gentle touch on her back as an assault. At the same time Annie realized that yoga might offer her a way to liberate herself from the constant sense of danger that she felt in her body. With my encouragement she returned the following week.
Annie had always found it easier to write about her experiences than to talk about them. After her second yoga class she wrote to me: “I don’t know all of the reasons that yoga terrifies me so much, but I do know that it will be an incredible source of healing for me and that is why I am working on myself to try it. Yoga is about looking inward instead of outward and listening to my body, and a lot of my survival has been geared around never doing those things. Going to the class today my heart was racing and part of me really wanted to turn around, but then I just kept putting one foot in front of the other until I got to the door and went in. After the class I came home and slept for four hours. This week I tried doing yoga at home and the words came to me ‘Your body has things to say.’ I said back to myself, ‘I will try and listen.’”
A few days later Annie wrote: “Some thoughts during and after yoga today. It occurred to me how disconnected I must be from my body when I cut it. When I was doing the poses I noticed that my jaw and the whole area from where my legs end to my bellybutton is where I am tight, tense and holding the pain and memories. Sometimes you have asked me where I feel things and I can’t even begin to locate them, but today I felt those places very clearly and it made me want to cry in a gentle kind of way.”
The following month both of us went on vacation and, invited to stay in touch, Annie wrote to me again: “I’ve been doing yoga on my own in a room that overlooks the lake. I’m continuing to read the book you lent me [Stephen Cope’s wonderful Yoga and the Quest for the True Self]. It’s really interesting to think about how much I have been refusing to listen to my body, which is such an important part of who I am. Yesterday when I did yoga I thought about letting my body tell me the story it wants to tell and in the hip opening poses there was a lot of pain and sadness. I don’t think my mind is going to let really vivid images come up as long as I am away from home, which is good. I think now about how unbalanced I have been and about how hard I have tried to deny the past, which is a part of my true self. There is so much I can learn if I am open to it and then I won’t have to fight myself every minute of every day.”
One of the hardest yoga positions for Annie to tolerate was one that’s often called Happy Baby, in which you lie on your back with your knees deeply bent and the soles of your feet pointing to the ceiling, while holding your toes with your hands. This rotates the pelvis into a wide-open position. It’s easy to understand why this would make a rape victim feel extremely vulnerable. Yet, as long as Happy Baby (or any posture that resembles it) precipitates intense panic, it is difficult to be intimate. Learning how to comfortably assume Happy Baby is a challenge for many patients in our yoga classes.
GETTING TO KNOW ME: CULTIVATING INTEROCEPTION
One of the clearest lessons from contemporary neuroscience is that our sense of ourselves is anchored in a vital connection with our bodies.14 We do not truly know ourselves unless we can feel and interpret our physical sensations; we need to register and act on these sensations to navigate safely through life.15 While numbing (or compensatory sensation seeking) may make life tolerable, the price
you pay is that you lose awareness of what is going on inside your body and, with that, the sense of being fully, sensually alive.
In chapter 6 I discussed alexithymia, the technical term for not being able to identify what is going on inside oneself.16 People who suffer from alexithymia tend to feel physically uncomfortable but cannot describe exactly what the problem is. As a result they often have multiple vague and distressing physical complaints that doctors can’t diagnose. In addition, they can’t figure out for themselves what they’re really feeling about any given situation or what makes them feel better or worse. This is the result of numbing, which keeps them from anticipating and responding to the ordinary demands of their bodies in quiet, mindful ways. At the same time, it muffles the everyday sensory delights of experiences like music, touch, and light, which imbue life with value. Yoga turned out to be a terrific way to (re)gain a relationship with the interior world and with it a caring, loving, sensual relationship to the self.
If you are not aware of what your body needs, you can’t take care of it. If you don’t feel hunger, you can’t nourish yourself. If you mistake anxiety for hunger, you may eat too much. And if you can’t feel when you’re satiated, you’ll keep eating. This is why cultivating sensory awareness is such a critical aspect of trauma recovery. Most traditional therapies downplay or ignore the moment-to-moment shifts in our inner sensory world. But these shifts carry the essence of the organism’s responses: the emotional states that are imprinted in the body’s chemical profile, in the viscera, in the contraction of the striated muscles of the face, throat, trunk, and limbs.17 Traumatized people need to learn that they can tolerate their sensations, befriend their inner experiences, and cultivate new action patterns.
In yoga you focus your attention on your breathing and on your sensations moment to moment. You begin to notice the connection between your emotions and your body—perhaps how anxiety about doing a pose actually throws you off balance. You begin to experiment with changing the way you feel. Will taking a deep breath relieve that tension in your shoulder? Will focusing on your exhalations produce a sense of calm?18
Simply noticing what you feel fosters emotional regulation, and it helps you to stop trying to ignore what is going on inside you. As I often tell my students, the two most important phrases in therapy, as in yoga, are “Notice that” and “What happens next?” Once you start approaching your body with curiosity rather than with fear, everything shifts.
Body awareness also changes your sense of time. Trauma makes you feel as if you are stuck forever in a helpless state of horror. In yoga you learn that sensations rise to a peak and then fall. For example, if an instructor invites you to enter a particularly challenging position, you may at first feel a sense of defeat or resistance, anticipating that you won’t be able to tolerate the feelings brought up by this particular position. A good yoga teacher will encourage you to just notice any tension while timing what you feel with the flow of your breath: “We’ll be holding this position for ten breaths.” This helps you anticipate the end of discomfort and strengthens your capacity to deal with physical and emotional distress. Awareness that all experience is transitory changes your perspective on yourself.
This is not to say that regaining interoception isn’t potentially upsetting. What happens when a newly accessed feeling in your chest is experienced as rage, or fear, or anxiety? In our first yoga study we had a 50 percent dropout rate, the highest of any study we’d ever done. When we interviewed the patients who’d left, we learned that they had found the program too intense: Any posture that involved the pelvis could precipitate intense panic or even flashbacks to sexual assaults. Intense physical sensations unleashed the demons from the past that had been so carefully kept in check by numbing and inattention. This taught us to go slow, often at a snail’s pace. That approach paid off: In our most recent study only one out of thirty-four participants did not finish.
Effects of a weekly yoga class. After twenty weeks, chronically traumatized women developed increased activation of critical brain structures involved in self-regulation: the insula and the medial prefrontal cortex.
YOGA AND THE NEUROSCIENCE OF SELF-AWARENESS
During the past few years brain researchers such as my colleagues Sara Lazar and Britta Hölzel at Harvard have shown that intensive meditation has a positive effect on exactly those brain areas that are critical for physiological self-regulation.19 In our latest yoga study, with six women with histories of profound early trauma, we also found the first indications that twenty weeks of yoga practice increased activation of the basic self-system, the insula and the medial prefrontal cortex (see chapter 6). This research needs much more work, but it opens up new perspectives on how actions that involve noticing and befriending the sensations in our bodies can produce profound changes in both mind and brain that can lead to healing from trauma.
After each of our yoga studies, we asked the participants what effect the classes had had on them. We never mentioned the insula or interoception; in fact, we kept the discussion and explanation to a minimum so that they could focus inward.
Here is a sample of their responses:
“My emotions feel more powerful. Maybe it’s just that I can recognize them now.”
“I can express my feelings more because I can recognize them more.
I feel them in my body, recognize them, and address them.”
“I now see choices, multiple paths. I can decide and I can choose my life, it doesn’t have to be repeated or be experienced like a child.” “I was able to move my body and be in my body in a safe place and without hurting myself/getting hurt.”
LEARNING TO COMMUNICATE
People who feel safe in their bodies can begin to translate the memories that previously overwhelmed them into language. After Annie had been practicing yoga three times a week for about a year, she noticed that she was able to talk much more freely to me about what had happened to her. She thought this almost miraculous. One day, when she knocked over a glass of water, I got up from my chair and approached her with a Kleenex box, saying, “Let me clean that up.” This precipitated a brief, intense panic reaction. She was quickly able to contain herself, though, and explained why those particular words were so upsetting to her—they were what her father would say after he’d raped her. Annie wrote to me after that session: “Did you notice that I have been able to say the words out loud? I didn’t have to write them down to tell you what was happening. I didn’t lose trust in you because you said words that triggered me. I understood that the words were a trigger and not terrible words that no one should say.”
Annie continues to practice yoga and to write to me about her experiences: “Today I went to a morning yoga class at my new yoga studio. The teacher talked about breathing to the edge of where we can and then noticing that edge. She said that if we notice our breath we are in the present because we can’t breathe in the future or the past. It felt so amazing to me to be practicing breathing in that way after we had just talked about it, like I had been given a gift. Some of the poses can be triggering for me. Two of them were today, one where your legs are up frog like and one where you are doing really deep breathing into your pelvis. I felt the beginning of panic, especially in the
breathing pose, like oh no that’s not a part of my body I want to feel. But then I was able to stop myself and just say, notice that this part of your body is holding experiences and then just let it go. You don’t have to stay there but you don’t have to leave either, just use it as information. I don’t know that I have ever been able to do that in such a conscious way before. It made me think that if I notice without being so afraid, it will be easier for me to believe myself.”
In another message, Annie reflected on the changes in her life: “I slowly learned to just have my feelings, without being hijacked by them. Life is more manageable: I am more attuned to my day and more present in the moment. I am more tolerant of physical touch. My husband and I are enjoying watching movies cuddled together in bed. . . a huge step. All this helped me finally feel intimate with my husband.”
CHAPTER 13: HEALING FROM TRAUMA: OWNING YOUR SELF
1.“Self-leadership” is the term used by Dick Schwartz in internal family system therapy, the topic of chapter 17.
2.The exceptions are Pesso’s and Schwartz’s work, detailed in chapters 17 and 18, which I practice, and from which I have personally benefited, but which I have not studied scientifically—at least not yet.
3.A. F. Arnsten, “Enhanced: The Biology of Being Frazzled,” Science 280, no. 5370 (1998): 1711–12; A. Arnsten, “Stress Signalling Pathways That Impair Prefrontal Cortex Structure and Function,” Nature Reviews Neuroscience 10, no. 6 (2009): 410–22.
4.D. J. Siegel, The Mindful Therapist: A Clinician’s Guide to Mindsight and Neural Integration (New York: WW Norton, 2010).
5.J. E. LeDoux, “Emotion Circuits in the Brain,” Annual Review of Neuroscience 23, no. 1 (2000): 155– 84. See also M. A. Morgan, L. M. Romanski, and J. E. LeDoux, “Extinction of Emotional Learning: Contribution of Medial Prefrontal Cortex,” Neuroscience Letters 163, no. 1 (1993): 109–113; and J. M. Moscarello and J. E. LeDoux, “Active Avoidance Learning Requires Prefrontal Suppression of Amygdala-Mediated Defensive Reactions,” Journal of Neuroscience 33, no. 9 (2013): 3815–23.
6.S. W. Porges, “Stress and Parasympathetic Control,” Stress Science: Neuroendocrinology 306 (2010). See also S. W. Porges, “Reciprocal Influences Between Body and Brain in the Perception and Expression of Affect,” in The Healing Power of Emotion: Affective Neuroscience, Development & Clinical Practice, Norton Series on Interpersonal Neurobiology (New York: WW Norton, 2009), 27.
7.B. A. van der Kolk, et al., “Yoga As an Adjunctive Treatment for PTSD.” Journal of Clinical Psychiatry 75, no. 6 (June 2014): 559–65.
8.Sebern F. Fisher, Neurofeedback in the Treatment of Developmental Trauma: Calming the Fear-Driven Brain. (New York: WW Norton & Company, 2014).
9.R. P. Brown and P. L. Gerbarg, “Sudarshan Kriya Yogic Breathing in the Treatment of Stress, Anxiety, and Depression—Part II: Clinical Applications and Guidelines,” Journal of Alternative & Complementary Medicine 11, no. 4 (2005): 711–17. See also C. L. Mandle, et al., “The Efficacy of Relaxation Response Interventions with Adult Patients: A Review of the Literature,” Journal of Cardiovascular Nursing 10 (1996): 4–26; and M. Nakao, et al., “Anxiety Is a Good Indicator for Somatic Symptom Reduction Through Behavioral Medicine Intervention in a Mind/Body Medicine Clinic,” Psychotherapy and Psychosomatics 70 (2001): 50–57.
10.C. Hannaford, Smart Moves: Why Learning Is Not All in Your Head (Arlington, VA: Great Ocean Publishers, 1995), 22207–3746.
11.J. Kabat-Zinn, Full Catastrophe Living: Using the Wisdom of Your Body and Mind to Face Stress, Pain, and Illness (New York: Bantam Books, 2013). See also D. Fosha, D. J. Siegel, and M. Solomon, eds., The Healing Power of Emotion: Affective Neuroscience, Development & Clinical Practice, Norton Series on Interpersonal Neurobiology (New York: WW Norton, 2011); and B. A. van der Kolk, “Posttraumatic Therapy in the Age of Neuroscience,” Psychoanalytic Dialogues 12, no. 3 (2002): 381– 92.
12.As we have seen in chapter 5, brain scans of people suffering from PTSD show altered activation in areas associated with the default network, which is involved with autobiographical memory and a continuous sense of self.
13.P. A. Levine, In an Unspoken Voice: How the Body Releases Trauma and Restores Goodness (Berkeley: North Atlantic, 2010).
14.P. Ogden, Trauma and the Body (New York: Norton, 2009). See also A. Y. Shalev, “Measuring Outcome in Posttraumatic Stress Disorder,” Journal of Clinical Psychiatry 61, supp. 5 (2000): 33–42.
15.I. Kabat-Zinn, Full Catastrophe Living. p. xx
16.S. G. Hofmann, et al., “The Effect of Mindfulness-Based Therapy on Anxiety and Depression: A Meta-Analytic Review,” Journal of Consulting and Clinical Psychology 78, no.2 (2010): 169–83; J. D. Teasdale, et al., “Prevention of Relapse/Recurrence in Major Depression by Mindfulness-Based Cognitive Therapy,” Journal of Consulting and Clinical Psychology 68 (2000): 615–23. See also Britta K. Hölzel, et al., “How Does Mindfulness Meditation Work? Proposing Mechanisms of Action from a Conceptual and Neural Perspective.” Perspectives on Psychological Science 6, no. 6 (2011): 537–59; and P. Grossman, et al., “Mindfulness-Based Stress Reduction and Health Benefits: A Meta-Analysis,” Journal of Psychosomatic Research 57, no. 1 (2004): 35–43.
17.The brain circuits involved in mindfulness meditation have been well established, and improve attention regulation and has a positive effect on the interference of emotional reactions with attentional performance tasks. See L. E. Carlson, et al., “One Year Pre-Post Intervention Follow-up of Psychological, Immune, Endocrine and Blood Pressure Outcomes of Mindfulness-Based Stress Reduction (MBSR) in Breast and Prostate Cancer Outpatients,” Brain, Behavior, and Immunity 21, no. 8 (2007): 1038–49; and R. J. Davidson, et al., “Alterations in Brain and Immune Function Produced by Mindfulness Meditation,” Psychosomatic Medicine 65, no. 4 (2003): 564–70.
18.Britta Hölzel and her colleagues have done extensive research on meditation and brain function and have shown that it involves the dorsomedial PFC, ventrolateral PFC, and rostral anterior congulate (ACC). See B. K. Hölzel, et al., “Stress Reduction Correlates with Structural Changes in the Amygdala,” Social Cognitive and Affective Neuroscience 5 (2010): 11–17; B. K. Hölzel, et al., “Mindfulness Practice Leads to Increases in Regional Brain Gray Matter Density,” Psychiatry Research 191, no. 1 (2011): 36–43; B. K. Hölzel, et al., “Investigation of Mindfulness Meditation Practitioners with Voxel-Based Morphometry,” Social Cognitive and Affective Neuroscience 3, no. 1 (2008): 55–61; and B. K. Hölzel, et al., “Differential Engagement of Anterior Cingulate and Adjacent Medial Frontal Cortex in Adept Meditators and Non-meditators,” Neuroscience Letters 421, no. 1 (2007): 16–21.
19.The main brain structure involved in body awareness is the anterior insula. See A. D. Craig, “Interoception: The Sense of the Physiological Condition of the Body,” Current Opinion on Neurobiology 13 (2003): 500–505; Critchley, Wiens, Rotshtein, Ohman, and Dolan, 2004; N. A. S Farb, Z. V. Segal, H. Mayberg, J. Bean, D. McKeon, Z. Fatima, et al., “Attending to the Present: Mindfulness Meditation Reveals Distinct Neural Modes of Self-Reference,” Social Cognitive and Affective Neuroscience 2 (2007): 313–22.; J. A. Grant, J. Courtemanche, E. G. Duerden, G. H. Duncan, and P. Rainville, (2010). “Cortical Thickness and Pain Sensitivity in Zen Meditators,” Emotion 10, no. 1 (2010): 43–53.
20.S. J. Banks, et al., “Amygdala-Frontal Connectivity During Emotion-Regulation,” Social Cognitive and Affective Neuroscience 2, no. 4 (2007): 303–12. See also M. R. Milad, et al., “Thickness of Ventromedial Prefrontal Cortex in Humans Is Correlated with Extinction Memory,” Proceedings of the National Academy of Sciences of the United States of America 102, no. 30 (2005): 10706–11; and S. L. Rauch, L. M. Shin, and E. A. Phelps, “Neurocircuitry Models of Posttraumatic Stress Disorder and Extinction: Human Neuroimaging Research—Past, Present, and Future,” Biological Psychiatry 60, no. 4 (2006): 376–82.
21.A. Freud and D. T. Burlingham. War and Children (New York University Press, 1943).
22.There are three different ways in which people deal with overwhelming experiences: dissociation (spacing out, shutting down), depersonalization (feeling like it’s not you it’s happening to), and derealization (feeling like whatever is happening is not real).
23.My colleagues at the Justice Resource Institute created a residential treatment program for adolescents, The van der Kolk Center at Glenhaven Academy, that implements many of the trauma-informed treatments discussed in this book, including yoga, sensory integration, neurofeedback and theater. http://www.jri.org/vanderkolk/about. The overarching treatment model, attachment, self-regulation, and competency (ARC), was developed by my colleagues Margaret Blaustein and Kristine
Kinneburgh. Margaret E. Blaustein, and Kristine M. Kinniburgh, Treating Traumatic Stress in Children and Adolescents: How to Foster Resilience Through Attachment, Self-Regulation, and Competency (New York: Guilford Press, 2012).
24.C. K. Chandler, Animal Assisted Therapy in Counseling (New York: Routledge, 2011). See also A. J. Cleveland, “Therapy Dogs and the Dissociative Patient: Preliminary Observations,” Dissociation 8, no. 4 (1995): 247–52; and A. Fine, Handbook on Animal Assisted Therapy: Theoretical Foundations and Guidelines for Practice (San Diego: Academic Press, 2010).
25.E. Warner, et al., “Can the Body Change the Score? Application of Sensory Modulation Principles in the Treatment of Traumatized Adolescents in Residential Settings,” Journal of Family Violence 28, no. 7 (2013): 729–38. See also A. J. Ayres, Sensory Integration and Learning Disorders (Los Angeles: Western Psychological Services, 1972); H. Hodgdon, et al., “Development and Implementation of Trauma-Informed Programming in Residential Schools Using the ARC Framework,” Journal of Family Violence 27, no. 8 (2013); J. LeBel, et al., “Integrating Sensory and Trauma-Informed Interventions: A Massachusetts State Initiative, Part 1,” Mental Health Special Interest Section Quarterly 33, no. 1 (2010): 1–4;
26.They appeared to have activated the vestibule-cerebellar system in the brain, which seems to be involved in self-regulation and can be damaged by early neglect.
27.Aaron R. Lyon and Karen S. Budd, “A Community Mental Health Implementation of Parent–Child Interaction Therapy (PCIT).” Journal of Child and Family Studies 19, no. 5 (2010): 654–68. See also Anthony J. Urquiza and Cheryl Bodiford McNeil, “Parent-Child Interaction Therapy: An Intensive Dyadic Intervention for Physically Abusive Families.” Child Maltreatment 1, no 2 (1996): 134–44; J. Borrego Jr., et al. “Research Publications.” Child and Family Behavior Therapy 20: 27-54.
28.B. A. van der Kolk, et al., “Fluoxetine in Post Traumatic Stress,” Journal of Clinical Psychiatry (1994): 517–22.
29.P. Ogden, K. Minton, and C. Pain, Trauma and the Body (New York, Norton, 2010); P. Ogden and J. Fisher, Sensorimotor Psychotherapy: Interventions for Trauma and Attachment (New York: Norton, 2014).
30.P. Levine, In an Unspoken Voice (Berkeley: North Atlantic Books); P. Levine, Waking the Tiger (Berkeley: North Atlantic Books).
31.For more on impact model mugging, see http://modelmugging.org/.
32.S. Freud, Remembering, Repeating, and Working Through (Further Recommendations on the Technique of Psychoanalysis II), standard ed. (London: Hogarth Press, 1914), p. 371
33.E. Santini, R. U. Muller, and G. J. Quirk, “Consolidation of Extinction Learning Involves Transfer from NMDA-Independent to NMDA-Dependent Memory,” Journal of Neuroscience 21 (2001): 9009– 17.
34.E. B. Foa and M. J. Kozak, “Emotional Processing of Fear: Exposure to Corrective Information,” Psychological Bulletin 99, no. 1 (1986): 20–35.
35.C. R. Brewin, “Implications for Psychological Intervention,” in Neuropsychology of PTSD: Biological, Cognitive, and Clinical Perspectives, ed. J. J. Vasterling and C. R. Brewin (New York: Guilford, 2005), 272.
36.T. M. Keane, “The Role of Exposure Therapy in the Psychological Treatment of PTSD,” National Center for PTSD Clinical Quarterly 5, no. 4 (1995): 1–6.
37.E. B. Foa and R. J. McNally, “Mechanisms of Change in Exposure Therapy,” in Current Controversies in the Anxiety Disorders, ed. R. M. Rapee (New York: Guilford, 1996), 329–43.
38.J. D. Ford and P. Kidd, “Early Childhood Trauma and Disorders of Extreme Stress as Predictors of Treatment Outcome with Chronic PTSD,” Journal of Traumatic Stress 18 (1998): 743–61. See also A. McDonagh-Coyle, et al., “Randomized Trial of Cognitive-Behavioral Therapy for Chronic Posttraumatic Stress Disorder in Adult Female Survivors of Childhood Sexual Abuse,” Journal of Consulting and Clinical Psychology 73, no. 3 (2005): 515–24; Institute of Medicine of the National Academies, Treatment of Posttraumatic Stress Disorder: An Assessment of the Evidence (Washington:
National Academies Press, 2008); and R. Bradley, et al., “A Multidimensional Meta-Analysis of Psychotherapy for PTSD,” American Journal of Psychiatry 162, no. 2 (2005): 214–27.
39.J. Bisson, et al., “Psychological Treatments for Chronic Posttraumatic Stress Disorder: Systematic Review and Meta-Analysis,” British Journal of Psychiatry 190 (2007): 97–104. See also L. H. Jaycox, E. B. Foa, and A. R. Morrall, “Influence of Emotional Engagement and Habituation on Exposure Therapy for PTSD,” Journal of Consulting and Clinical Psychology 66 (1998): 185–92.
40.“Dropouts: in prolonged exposure (n = 53 [38%]); in present-centered therapy (n = 30 [21%]) (P = .002). The control group also had a high rate of casualties: 2 nonsuicidal deaths, 9 psychiatric hospitalizations, and 3 suicide attempts.” P. P. Schnurr, et al., “Cognitive Behavioral Therapy for Posttraumatic Stress Disorder in Women,” JAMA 297, no. 8 (2007): 820–30.
41.R. Bradley, et al., “A Multidimensional Meta-Analysis of Psychotherapy for PTSD,” American Journal of Psychiatry 162, no. 2 (2005): 214–27.
42.J. H. Jaycox and E. B. Foa, “Obstacles in Implementing Exposure Therapy for PTSD: Case Discussions and Practical Solutions,” Clinical Psychology and Psychotherapy 3, no. 3 (1996): 176–84. See also E. B. Foa, D. Hearst-Ikeda, and K. J. Perry, “Evaluation of a Brief Cognitive-Behavioral Program for the Prevention of Chronic PTSD in Recent Assault Victims,” Journal of Consulting and Clinical Psychology 63 (1995): 948–55.
43.Alexander McFarlane personal communication.
44.R. K. Pitman, et al., “Psychiatric Complications During Flooding Therapy for Posttraumatic Stress Disorder,” Journal of Clinical Psychiatry 52, no. 1 (January 1991): 17–20.
45.Jean Decety, Kalina J. Michalska, and Katherine D. Kinzler, “The Contribution of Emotion and Cognition to Moral Sensitivity: A Neurodevelopmental Study,” Cerebral Cortex 22 no. 1 (2012): 209– 20; Jean Decety, C. Daniel Batson, “Neuroscience Approaches to Interpersonal Sensitivity,” 2, nos. 3-4 (2007).
46.K. H. Seal, et al., “VA Mental Health Services Utilization in Iraq and Afghanistan Veterans in the First Year of Receiving New Mental Health Diagnoses,” Journal of Traumatic Stress 23 (2010): 5–16.
47.L. Jerome, “(+/-)-3,4-Methylenedioxymethamphetamine (MDMA, “Ecstasy”) Investigator’s Brochure,” December 2007, available at www.maps.org/research/mdma/protocol/ib_mdma_new08.pdf (accessed August 16, 2012).
48.John H. Krystal, et al. “Chronic 3, 4-methylenedioxymethamphetamine (MDMA) use: effects on mood and neuropsychological function?.” The American Journal of Drug and Alcohol Abuse 18.3 (1992): 331-341.
49.Mithoefer, Michael C., et al., “The safety and efficacy of±3, 4-methylenedioxymethamphetamine-assisted psychotherapy in subjects with chronic, treatment-resistant posttraumatic stress disorder: the first randomized controlled pilot study.” Journal of Psychopharmacology 25.4 (2011): 439-452; M. C. Mithoefer, et al., “Durability of Improvement in Posttraumatic Stress Disorder Symptoms and Absence of Harmful Effects or Drug Dependency after 3, 4-Methylenedioxymethamphetamine-Assisted Psychotherapy: A Prospective Long-Term Follow-up Study,” Journal of Psychopharmacology 27, no. 1 (2013): 28–39.
50.J. D. Bremner, “Neurobiology of Posttraumatic Stress Disorder,” in Posttraumatic Stress Disorder: A Critical Review, ed. R. S. Rynoos (Lutherville, MD: Sidran Press, 1994), 43–64.
51.http://cdn.nextgov.com/nextgov/interstitial.html?
v=2.1.1&rf=http%3A%2F%2Fwww.nextgov.com%2Fhealth%2F2011%2F01%2Fmilitarys-drug-policy-threatens-troops-health-doctors-say%2F48321%2F.
39. J. R. T. Davidson, “Drug Therapy of Posttraumatic Stress Disorder,” British Journal of Psychiatry 160 (1992): 309–314. See also R. Famularo, R. Kinscherff, and T. Fenton, “Propranolol Treatment for Childhood Posttraumatic Stress Disorder Acute Type,” American Journal of Disorders of Childhood 142 (1988): 1244–47; F. A. Fesler, “Valproate in Combat-Related Posttraumatic Stress Disorder,” Journal of Clinical Psychiatry 52 (1991): 361–64; B. H. Herman, et al., “Naltrexone Decreases Self-Injurious Behavior,” Annals of Neurology 22 (1987): 530–34; and B. A. van der Kolk, et al.,
“Fluoxetine in Posttraumatic Stress Disorder.”
53.B. Van der Kolk, et al., “A Randomized Clinical Trial of EMDR, Fluoxetine and Pill Placebo in the Treatment of PTSD: Treatment Effects and Long-Term Maintenance,” Journal of Clinical Psychiatry 68 (2007): 37–46.
54.R. A. Bryant, et al., “Treating Acute Stress Disorder: An Evaluation of Cognitive Behavior Therapy and Supportive Counseling Techniques,” American Journal of Psychiatry 156, no. 11 (November 1999): 1780–86; N. P. Roberts et al., “Early Psychological Interventions to Treat Acute Traumatic Stress Symptoms,” Cochran Database of Systematic Reviews 3 (March 2010).
55.This includes the alpha1 receptor antagonist prazosin, the alpha2 receptor antagonist clonidine, and
the beta receptor antagonist propranolol. See M. J. Friedman and J. R. Davidson, “Pharmacotherapy for PTSD,” in Handbook of PTSD: Science and Practice, ed. M. J. Friedman, T. M. Keane, and P. A. Resick (New York: Guilford Press, (2007), 376.
53. M. A. Raskind, et al., “A Parallel Group Placebo Controlled Study of Prazosin for Trauma Nightmares and Sleep Disturbance in Combat Veterans with Posttraumatic Stress Disorder,” Biological Psychiatry 61, no. 8 (2007): 928–34. F. B. Taylor, et al., “Prazosin Effects on Objective Sleep Measures and Clinical Symptoms in Civilian Trauma Posttraumatic Stress Disorder: A Placebo-Controlled Study,” Biological Psychiatry 63, no. 6 (2008): 629–32.
Lithium, lamotrigin, carbamazepine, divalproex, gabapentin, and topiramate may help to control trauma-related aggression and irritability. Valproate has been shown to be effective in several case reports with PTSD, including with military veteran patients with chronic PTSD. Friedman and Davidson, “Pharmacotherapy for PTSD”; F. A. Fesler, “Valproate in Combat-Related Posttraumatic Stress Disorder,” Journal of Clinical Psychiatry 52, no. 9 (1991): 361–64. The following study showed a 37.4 percent reduction in PTSD S. Akuchekian and S. Amanat, “The Comparison of Topiramate and Placebo in the Treatment of Posttraumatic Stress Disorder: A Randomized, Double-Blind Study,” Journal of Research in Medical Sciences 9, no. 5 (2004): 240–44.
G. Bartzokis, et al., “Adjunctive Risperidone in the Treatment of Chronic Combat-Related Posttraumatic Stress Disorder,” Biological Psychiatry 57, no. 5 (2005): 474–79. See also D. B. Reich, et al., “A Preliminary Study of Risperidone in the Treatment of Posttraumatic Stress Disorder Related to Childhood Abuse in Women,” Journal of Clinical Psychiatry 65, no. 12 (2004): 1601–1606.
The other methods include interventions that usually help traumatized individuals sleep, like the antidepressant trazodone, binaural beat apps, light/sound machines like Proteus (www.brainmachines.com), HRV monitors like hearthmath (http://www.heartmath.com/), and iRest, an effective yoga-based intervention. (http://www.irest.us/)
D. Wilson, “Child’s Ordeal Shows Risks of Psychosis Drugs for Young,” New York Times, September 1, 2010, available at http://www.nytimes.com/2010/09/02/business/02kids.html? pagewanted=all&_r=0.
M. Olfson, et al., “National Trends in the Office-Based Treatment of Children, Adolescents, and Adults with Antipsychotics,” Archives of General Psychiatry 69, no. 12 (2012): 1247–56.
E. Harris, et al., “Perspectives on Systems of Care: Concurrent Mental Health Therapy Among Medicaid-Enrolled Youths Starting Antipsychotic Medications,” FOCUS 10, no. 3 (2012): 401–407.
B. A. Van der Kolk, “The Body Keeps the Score: Memory and the Evolving Psychobiology of Posttraumatic Stress,” Harvard Review of Psychiatry 1, no. 5 (1994): 253–65.
B. Brewin, “Mental Illness is the Leading Cause of Hospitalization for Active-Duty Troops,” Nextgov.com, May 17, 2012, http://www.nextgov.com/health/2012/05/mental-illness-leading-cause-hospitalization-active-duty-troops/55797/.
Mental health drug expenditures, Department of Veterans affairs. http://www.veterans.senate.gov/imo/media/doc/For%20the%20Record%20-%20CCHR%204.30.14.pdf.
CHAPTER 14: LANGUAGE: MIRACLE AND TYRANNY
1.Dr. Spencer Eth to Bessel A. van der Kolk, March 2002.
2.J. Breuer and S. Freud, “The Physical Mechanisms of Hysterical Phenomena,” in The Standard Edition of the Complete Psychological Works of Sigmund Freud (London: Hogarth Press, 1893). J. Breuer and S. Freud, Studies on Hysteria (New York: Basic Books, 2009).
3.T. E. Lawrence, Seven Pillars of Wisdom (New York: Doubleday, 1935).
4.E. B. Foa, et al., “The Posttraumatic Cognitions Inventory (PTCI): Development and Validation,” Psychological Assessment 11, no. 3 (1999): 303–314.
5.K. Marlantes, What It Is Like to Go to War (New York: Grove Press, 2011).
6.Ibid., 114.
7.Ibid., 129.
8.H. Keller, The World I Live In (1908), ed. R. Shattuck (New York: NYRB Classics, 2004). See also R. Shattuck, “A World of Words,” New York Review of Books, February 26, 2004.
9.H. Keller, The Story of My Life, ed. R. Shattuck and D. Herrmann (New York: Norton, 2003).
10.W. M. Kelley, et al., “Finding the Self? An Event-Related fMRI Study,” Journal of Cognitive Neuroscience 14, no. 5 (2002): 785–94. See also N. A. Farb, et al., “Attending to the Present: Mindfulness Meditation Reveals Distinct Neural Modes of Self-Reference,” Social Cognitive and Affective Neuroscience 2, no. 4 (2007): 313–22. P. M. Niedenthal, “Embodying Emotion,” Science 316, no. 5827 (2007): 1002–1005; and J. M. Allman, “The Anterior Cingulate Cortex,” Annals of the New York Academy of Sciences 935, no. 1 (2001): 107–117.
11.J. Kagan, dialogue with the Dalai Lama, Massachusetts Institute of Technology, 2006. http://www.mindandlife.org/about/history/.
12.A. Goldman and F. de Vignemont, “Is Social Cognition Embodied?” Trends in Cognitive Sciences 13, no. 4 (2009): 154–59. See also A. D. Craig, “How Do You Feel—Now? The Anterior Insula and Human Awareness,” Nature Reviews Neuroscience 10 (2009): 59–70; H. D. Critchley, “Neural Mechanisms of Autonomic, Affective, and Cognitive Integration,” Journal of Comparative Neurology 493, no. 1 (2005): 154–66; T. D. Wager, et al., “Prefrontal-Subcortical Pathways Mediating Successful Emotion Regulation,” Neuron 59, no. 6 (2008): 1037–50; K. N. Ochsner, et al., “Rethinking Feelings: An fMRI Study of the Cognitive Regulation of Emotion,” Journal of Cognitive Neuroscience 14, no. 8 (2002): 1215–29; A. D’Argembeau, et al., “Self-Reflection Across Time: Cortical Midline Structures Differentiate Between Present and Past Selves,” Social Cognitive and Affective Neuroscience 3, no. 3 (2008): 244–52; Y. Ma, et al., “Sociocultural Patterning of Neural Activity During Self-Reflection,” Social Cognitive and Affective Neuroscience 9, no. 1 (2014): 73–80; R. N. Spreng, R. A. Mar, and A. S. Kim, “The Common Neural Basis of Autobiographical Memory, Prospection, Navigation, Theory of Mind, and the Default Mode: A Quantitative Meta-Analysis,” Journal of Cognitive Neuroscience 21, no. 3 (2009): 489–510; H. D. Critchley, “The Human Cortex Responds to an Interoceptive Challenge,” Proceedings of the National Academy of Sciences of the United States of America 101, no. 17 (2004): 6333–34; and C. Lamm, C. D. Batson, and J. Decety, “The Neural Substrate of Human Empathy: Effects of Perspective-Taking and Cognitive Appraisal,” Journal of Cognitive Neuroscience 19, no. 1 (2007): 42–58.
13.J. W. Pennebaker, Opening Up: The Healing Power of Expressing Emotions (New York: Guilford Press, 2012), 12.
14.Ibid., p. 19.
15.Ibid., p.35.
16.Ibid., p. 50.
17.J. W. Pennebaker, J. K. Kiecolt-Glaser, and R. Glaser, “Disclosure of Traumas and Immune Function: Health Implications for Psychotherapy,” Journal of Consulting and Clinical Psychology 56, no. 2 (1988): 239–45.
18.D. A. Harris, “Dance/Movement Therapy Approaches to Fostering Resilience and Recovery Among African Adolescent Torture Survivors,” Torture 17, no. 2 (2007): 134–55; M. Bensimon, D. Amir, and Y. Wolf, “Drumming Through Trauma: Music Therapy with Posttraumatic Soldiers,” Arts in Psychotherapy 35, no. 1 (2008): 34–48; M. Weltman, “Movement Therapy with Children Who Have Been Sexually Abused,” American Journal of Dance Therapy 9, no. 1 (1986): 47–66; H. Englund, “Death, Trauma and Ritual: Mozambican Refugees in Malawi,” Social Science & Medicine 46, no. 9 (1998): 1165–74; H. Tefferi, Building on Traditional Strengths: The Unaccompanied Refugee Children from South Sudan (1996); D. Tolfree, Restoring Playfulness: Different Approaches to Assisting Children Who Are Psychologically Affected by War or Displacement (Stockholm: Rädda Barnen, 1996), 158–73; N. Boothby, “Mobilizing Communities to Meet the Psychosocial Needs of Children in War and Refugee Crises,” in Minefields in Their Hearts: The Mental Health of Children in War and Communal Violence, ed. R. Apfel and B. Simon (New Haven, Yale Universit Press, 1996), 149–64; S. Sandel, S. Chaiklin, and A. Lohn, Foundations of Dance/Movement Therapy: The Life and Work of Marian Chace (Columbia, MD: American Dance Therapy Association, 1993); K. Callaghan, “Movement Psychotherapy with Adult Survivors of Political Torture and Organized Violence,” Arts in Psychotherapy 20, no. 5 (1993): 411–21; A. E. L. Gray, “The Body Remembers: Dance Movement Therapy with an Adult Survivor of Torture,” American Journal of Dance Therapy 23, no. 1 (2001): 29–43.
19.A. M. Krantz, and J. W. Pennebaker, “Expressive Dance, Writing, Trauma, and Health: When Words Have a Body.” Whole Person Healthcare 3 (2007): 201–29.
20.P. Fussell, The Great War and Modern Memory (London: Oxford University Press, 1975).
21.Theses findings have been replicated in the following studies: J. D. Bremner, “Does Stress Damage the Brain?” Biological Psychiatry 45, no. 7 (1999): 797–805; I. Liberzon, et al., “Brain Activation in PTSD in Response to Trauma-Related Stimuli,” Biological Psychiatry 45, no. 7 (1999): 817–26; L. M. Shin, et al., “Visual Imagery and Perception in Posttraumatic Stress Disorder: A Positron Emission Tomographic Investigation,” Archives of General Psychiatry 54, no. 3 (1997): 233–41; L. M. Shin, et al., “Regional Cerebral Blood Flow During Script-Driven Imagery in Childhood Sexual Abuse– Related PTSD: A PET Investigation,” American Journal of Psychiatry 156, no. 4 (1999): 575–84.
22.I am not sure if this term originated with me or with Peter Levine. I own a video where he credits me, but most of what I have learned about pendulation I’ve learned from him.
23.A small body of evidence offers support for claims that exposure/acupoints stimulation yields stronger outcomes and exposures strategies that incorporate conventional relaxation techniques. (www.vetcases.com). D. Church, et al., “Single-Session Reduction of the Intensity of Traumatic Memories in Abused Adolescents After EFT: A Randomized Controlled Pilot Study,” Traumatology 18, no. 3 (2012): 73–79; and D. Feinstein and D. Church, “Modulating Gene Expression Through Psychotherapy: The Contribution of Noninvasive Somatic Interventions,” Review of General Psychology 14, no. 4 (2010): 283–95.
24.T. Gil, et al., “Cognitive Functioning in Posttraumatic Stress Disorder,” Journal of Traumatic Stress 3, no. 1 (1990): 29–45; J. J. Vasterling, et al., “Attention, Learning, and Memory Performances and Intellectual Resources in Vietnam Veterans: PTSD and No Disorder Comparisons,” Neuropsychology 16, no. 1 (2002): 5.
25.In a neuroimaging study the PTSD subjects deactivated the speech area of their brain, Broca’s area, in response to neutral words. In other words: the decreased Broca’s area functioning that we had found in PTSD patients (see chapter 3) did not only occur in response to traumatic memories; it also happened when they were asked to pay attention to neutral words. This means that, as a group, traumatized
patients have a harder time to articulate what they feel and think about ordinary events. The PTSD group also had decreased activation of the medial prefrontal cortex (mPFC), the frontal lobe area that, as we have seen, conveys awareness of one’s self, and dampens activation of the amygdala, the smoke detector. This made it harder for them to suppress the brain’s fear response in response to a simple language task and again, made it harder to pay attention and go on with their lives. See: Moores, K. A., Clark, C. R., McFarlane, A. C., Brown, G. C., Puce, A., & Taylor, D. J. (2008). Abnormal recruitment of working memory updating networks during maintenance of trauma-neutral information in posttraumatic stress disorder. Psychiatry Research: Neuroimaging, 163(2), 156–170.
26.J. Breuer and S. Freud, “The Physical Mechanisms of Hysterical Phenomena,” in The Standard Edition of the Complete Psychological Works of Sigmund Freud (London: Hogarth Press, 1893).
27.D. L. Schacter, Searching for Memory (New York: Basic Books, 1996).
CHAPTER 15: LETTING GO OF THE PAST: EMDR
1. F. Shapiro, EMDR: The Breakthrough Eye Movement Therapy for Overcoming Anxiety, Stress, and Trauma (New York: Basic Books, 2004).
2. B. A. van der Kolk, et al., “A Randomized Clinical Trial of Eye Movement Desensitization and
Reprocessing (EMDR), Fluoxetine, and Pill Placebo in the Treatment of Posttraumatic Stress Disorder: Treatment Effects and Long-Term Maintenance,” Journal of Clinical Psychiatry 68, no. 1 (2007): 37– 46.
1. J. G. Carlson, et al., “Eye Movement Desensitization and Reprocessing (EDMR) Treatment for Combat-Related Posttraumatic Stress Disorder,” Journal of Traumatic Stress 11, no. 1 (1998): 3–24.
J. D. Payne, et al., “Sleep Increases False Recall of Semantically Related Words in the Deese-Roediger-McDermott Memory Task,” Sleep 29 (2006): A373.
B. A. van der Kolk and C. P. Ducey, “The Psychological Processing of Traumatic Experience: Rorschach Patterns in PTSD,” Journal of Traumatic Stress 2, no. 3 (1989): 259–74.
M. Jouvet, The Paradox of Sleep: The Story of Dreaming, trans. Laurence Garey (Cambridge, MA: MIT Press, 1999).
R. Greenwald, “Eye Movement Desensitization and Reprocessing (EMDR): A New Kind of Dreamwork?” Dreaming 5, no. 1 (1995): 51–55.
R. Cartwright, et al., “REM Sleep Reduction, Mood Regulation and Remission in Untreated Depression,” Psychiatry Research 121, no. 2 (2003): 159–67. See also R. Cartwright, et al., “Role of REM Sleep and Dream Affect in Overnight Mood Regulation: A Study of Normal Volunteers,” Psychiatry Research 81, no. 1 (1998): 1–8.
R. Greenberg, C. A. Pearlman, and D. Gampel, “War Neuroses and the Adaptive Function of REM Sleep,” British Journal of Medical Psychology 45, no. 1 1972): 27–33. Ramon Greenberg and Chester Pearlman, as well as our lab, found that traumatized veterans wake themselves up as soon as they enter a REM period. While many traumatized individuals use alcohol to help them sleep, they thereby keep themselves from the full benefits of dreaming (the integration and transformation of memory) and thereby may contribute to preventing the resolution of their PTSD.
B. van der Kolk, et al., “Nightmares and Trauma: A Comparison of Nightmares After Combat with Lifelong Nightmares in Veterans,” American Journal of Psychiatry 141, no. 2 (1984): 187–90.
N. Breslau, et al., “Sleep Disturbance and Psychiatric Disorders: A Longitudinal Epidemiological Study of Young Adults,” Biological Psychiatry 39, no. 6 (1996): 411–18.
R. Stickgold, et al., “Sleep-Induced Changes in Associative Memory,” Journal of Cognitive Neuroscience 11, no. 2 (1999): 182–93. See also R. Stickgold, “Of Sleep, Memories and Trauma,” Nature Neuroscience 10, no. 5 (2007): 540–42; and B. Rasch, et al., “Odor Cues During Slow-Wave Sleep Prompt Declarative Memory Consolidation,” Science 315, no. 5817 (2007): 1426–29.
E. J. Wamsley, et al., “Dreaming of a Learning Task Is Associated with Enhanced Sleep-Dependent Memory Consolidation,” Current Biology 20, no. 9, (May 11, 2010): 850–55.
14.R. Stickgold, “Sleep-Dependent Memory Consolidation,” Nature 437 (2005): 1272–78.
15.R. Stickgold, et al., “Sleep-Induced Changes in Associative Memory,” Journal of Cognitive Neuroscience 11, no. 2 (1999): 182–93.
16.J. Williams, et al., “Bizarreness in Dreams and Fantasies: Implications for the Activation-Synthesis Hypothesis,” Consciousness and Cognition 1, no. 2 (1992): 172–85. See also Stickgold, et al., “Sleep-Induced Changes in Associative Memory.”
17.M. P. Walker, et al., “Cognitive Flexibility Across the Sleep-Wake Cycle: REM-Sleep Enhancement of Anagram Problem Solving,” Cognitive Brain Research 14 (2002): 317–24.
18.R. Stickgold, “EMDR: A Putative Neurobiological Mechanism of Action,” Journal of Clinical Psychology 58 (2002): 61–75.
19.There are several studies on how eye movements help to process and transform traumatic memories. M. Sack, et al., “Alterations in Autonomic Tone During Trauma Exposure Using Eye Movement Desensitization and Reprocessing (EMDR)—Results of a Preliminary Investigation,” Journal of Anxiety Disorders 22, no. 7 (2008): 1264–71; B. Letizia, F. Andrea, and C. Paolo, Neuroanatomical Changes After Eye Movement Desensitization and Reprocessing (EMDR) Treatment in Posttraumatic Stress Disorder, The Journal of Neuropsychiatry and Clinical Neurosciences, 19, no. 4 (2007): 475–76; P. Levin, S. Lazrove, and B. van der Kolk, (1999). What Psychological Testing and Neuroimaging Tell Us About the Treatment of Posttraumatic Stress Disorder by Eye Movement Desensitization and Reprocessing, Journal of Anxiety Disorders, 13, nos. 1–2, 159–72; M. L. Harper, T. Rasolkhani Kalhorn, J. F. Drozd, “On the Neural Basis of EMDR Therapy: Insights from Qeeg Studies, Traumatology, 15, no. 2 (2009): 81–95; K. Lansing, D. G. Amen, C. Hanks, L. Rudy, “High-Resolution Brain SPECT Imaging and Eye Movement Desensitization and Reprocessing in Police Officers with PTSD,” The Journal of Neuropsychiatry and Clinical Neurosciences 17, no. 4 (2005): 526–32; T. Ohtani, K. Matsuo, K. Kasai, T. Kato, and N. Kato, “Hemodynamic Responses of Eye Movement Desensitization and Reprocessing in Posttraumatic Stress Disorder. Neuroscience Research, 65, no. 4 (2009): 375–83; M. Pagani, G. Högberg, D. Salmaso, D. Nardo, Ö. Sundin, C. Jonsson, and
T. Hällström, “Effects of EMDR Psychotherapy on 99mtc-HMPAO Distribution in Occupation-Related PostTraumatic Stress Disorder,” Nuclear Medicine Communications 28 (2007): 757–65; H. P. Söndergaard and U. Elofsson, “Psychophysiological Studies of EMDR,” Journal of EMDR Practice and Research 2, no. 4 (2008): 282–88.
CHAPTER 16: LEARNING TO INHABIT YOUR BODY: YOGA
1. Acupuncture and acupressure are widely practiced among trauma-oriented clinicians and is beginning to be systematically studied as a treatment for clinical PTSD. M. Hollifield, et al., “Acupuncture for Posttraumatic Stress Disorder: A Randomized Controlled Pilot Trial,” Journal of Nervous and Mental Disease 195, no. 6 (2007): 504–513. Studies that use fMRI to measure the effects of acupuncture on the areas of the brain associated with fear report acupuncture to produce rapid regulation of these brain regions. K. K. Hui, et al., “The Integrated Response of the Human Cerebro-Cerebellar and Limbic Systems to Acupuncture Stimulation at ST 36 as Evidenced by fMRI,” NeuroImage 27 (2005): 479– 96; J. Fang, et al., “The Salient Characteristics of the Central Effects of Acupuncture Needling: Limbic-Paralimbic-Neocortical Network Modulation,” Human Brain Mapping 30 (2009): 1196–206. D. Feinstein, “Rapid Treatment of PTSD: Why Psychological Exposure with Acupoint Tapping May Be Effective,” Psychotherapy: Theory, Research, Practice, Training 47, no. 3 (2010): 385–402; D. Church, et al., “Psychological Trauma Symptom Improvement in Veterans Using EFT (Emotional Freedom Technique): A Randomized Controlled Trial,” Journal of Nervous and Mental Disease 201 (2013): 153–60; D. Church, G. Yount, and A. J. Brooks, “The Effect of Emotional Freedom Techniques (EFT) on Stress Biochemistry: A Randomized Controlled Trial,” Journal of Nervous and Mental Disease 200 (2012): 891–96; R. P. Dhond, N. Kettner, and V. Napadow, “Neuroimaging Acupuncture Effects in the Human Brain,” Journal of Alternative and Complementary Medicine 13
(2007): 603–616; K. K. Hui, et al., “Acupuncture Modulates the Limbic System and Subcortical Gray Structures of the Human Brain: Evidence from fMRI Studies in Normal Subjects,” Human Brain Mapping 9 (2000): 13–25.
2. M. Sack, J. W. Hopper, and F. Lamprecht, “Low Respiratory Sinus Arrhythmia and Prolonged Psychophysiological Arousal in Posttraumatic Stress Disorder: Heart Rate Dynamics and Individual Differences in Arousal Regulation,” Biological Psychiatry 55, no. 3 (2004): 284–90. See also H. Cohen, et al., “Analysis of Heart Rate Variability in Posttraumatic Stress Disorder Patients in Response to a Trauma-Related Reminder,” Biological Psychiatry 44, no. 10 (1998): 1054–59; H. Cohen, et al., “Long-Lasting Behavioral Effects of Juvenile Trauma in an Animal Model of PTSD Associated with a Failure of the Autonomic Nervous System to Recover,” European Neuropsychopharmacology 17, no. 6 (2007): 464–77; and H. Wahbeh and B. S. Oken, “Peak High-Frequency HRV and Peak Alpha Frequency Higher in PTSD,” Applied Psychophysiology and Biofeedback 38, no. 1 (2013): 57–69.
3. J. W. Hopper, et al., “Preliminary Evidence of Parasympathetic Influence on Basal Heart Rate in Posttraumatic Stress Disorder,” Journal of Psychosomatic Research 60, no. 1 (2006): 83–90.
4. Arieh Shalev at Hadassah Medical School in Jerusalem and Roger Pitman’s experiments at Harvard also pointed in this direction: A. Y. Shalev, et al., “Auditory Startle Response in Trauma Survivors with Posttraumatic Stress Disorder: A Prospective Study,” American Journal of Psychiatry 157, no. 2 (2000): 255–61; R. K. Pitman, et al., “Psychophysiologic Assessment of Posttraumatic Stress Disorder Imagery in Vietnam Combat Veterans,” Archives of General Psychiatry 44, no. 11 (1987): 970–75; A. Y. Shalev, et al., “A Prospective Study of Heart Rate Response Following Trauma and the Subsequent Development of Posttraumatic Stress Disorder,” Archives of General Psychiatry 55, no. 6 (1998): 553– 59.
5. P. Lehrer, Y. Sasaki, and Y. Saito, “Zazen and Cardiac Variability,” Psychosomatic Medicine 61, no. 6 (1999): 812–21. See also R. Sovik, “The Science of Breathing: The Yogic View,” Progress in Brain Research 122 (1999): 491–505; P. Philippot, G. Chapelle, and S. Blairy, “Respiratory Feedback in the Generation of Emotion,” Cognition & Emotion 16, no. 5 (2002): 605–627; A. Michalsen, et al., “Rapid Stress Reduction and Anxiolysis Among Distressed Women as a Consequence of a Three-Month Intensive Yoga Program,” Medcal Science Monitor 11, no. 12 (2005): 555–61; G. Kirkwood et al., “Yoga for Anxiety: A Systematic Review of the Research Evidence,” British Journal of Sports Medicine 39 (2005): 884–91; K. Pilkington, et al., “Yoga for Depression: The Research Evidence,” Journal of Affective Disorders 89 (2005): 13–24; and P. Gerbarg and R. Brown, “Yoga: A Breath of Relief for Hurricane Katrina Refugees,” Current Psychiatry 4 (2005): 55–67.
6. B. Cuthbert et al., “Strategies of Arousal Control: Biofeedback, Meditation, and Motivation,” Journal of Experimental Psychology 110 (1981): 518–46. See also S. B. S. Khalsa, “Yoga as a Therapeutic Intervention: A Bibliometric Analysis of Published Research Studies,” Indian Journal of Physiology and Pharmacology 48 (2004): 269–85; M. M. Delmonte, “Meditation as a Clinical Intervention Strategy: A Brief Review,” International Journal of Psychosomatics 33 (1986): 9–12; I. Becker, “Uses of Yoga in Psychiatry and Medicine,” in Complementary and Alternative Medicine and Psychiatry, vol. 19, ed. P. R. Muskin PR (Washington: American Psychiatric Press, 2008); L. Bernardi, et al., “Slow Breathing Reduces Chemoreflex Response to Hypoxia and Hypercapnia, and Increases Baroreflex Sensitivity,” Journal of Hypertension 19, no. 12 (2001): 2221–29; R. P. Brown and P. L. Gerbarg, “Sudarshan Kriya Yogic Breathing in the Treatment of Stress, Anxiety, and Depression: Part I: Neurophysiologic Model,” Journal of Alternative and Complementary Medicine 11 (2005): 189– 201; R. P. Brown and P. L. Gerbarg, “Sudarshan Kriya Yogic Breathing in the Treatment of Stress, Anxiety, and Depression: Part II: Clinical Applications and Guidelines,” Journal of Alternative and Complementary Medicine 11 (2005): 711–17; C. C. Streeter, et al., “Yoga Asana Sessions Increase Brain GABA Levels: A Pilot Study,” Journal of Alternative and Complementary Medicine 13 (2007): 419–26; and C. C. Streeter, et al., “Effects of Yoga Versus Walking on Mood, Anxiety, and Brain GABA Levels: A Randomized Controlled MRS Study,” Journal of Alternative and Complementary Medicine 16 (2010): 1145–52.
7. There are dozens of scientific articles showing the positive effect of yoga for various medical conditions. The following is a small sample: S. B. Khalsa, “Yoga as a Therapeutic Intervention”; P. Grossman, et al., “Mindfulness-Based Stress Reduction and Health Benefits: A Meta-Analysis,” Journal of Psychosomatic Research 57 (2004): 35–43; K. Sherman, et al., “Comparing Yoga, Exercise, and a Self-Care Book for Chronic Low Back Pain: A Randomized, Controlled Trial,” Annals of Internal Medicine 143 (2005): 849–56; K. A. Williams, et al., “Effect of Iyengar Yoga Therapy for Chronic Low Back Pain,” Pain 115 (2005): 107–117; R. B. Saper, et al., “Yoga for Chronic Low Back Pain in a Predominantly Minority Population: A Pilot Randomized Controlled Trial,” Alternative Therapies in Health and Medicine 15 (2009): 18–27; J. W. Carson, et al., “Yoga for Women with Metastatic Breast Cancer: Results from a Pilot Study,” Journal of Pain and Symptom Management 33 (2007): 331–41.
8. B. A. van der Kolk, et al., “Yoga as an Adjunctive Therapy for PTSD,” Journal of Clinical Psychiatry 75, no. 6 (June 2014): 559–65.
9. A California company, HeartMath, has developed nifty devices and computer games that are both fun and effective in helping people to achieve better HRV. To date nobody has studied whether simple devices such as those developed by HeartMath can reduce PTSD symptoms, but this very likely the case. (see in www.heartmath.org.)
10.As of this writing there are twenty-four apps available on iTunes that claim to be able to help increase HRV, such as emWave, HeartMath, and GPS4Soul.
11.B. A. van der Kolk, “Clinical Implications of Neuroscience Research in PTSD,” Annals of the New York Academy of Sciences 1071, no. 1 (2006): 277–93.
12.S. Telles, et al., “Alterations of Auditory Middle Latency Evoked Potentials During Yogic Consciously Regulated Breathing and Attentive State of Mind,” International Journal of Psychophysiology 14, no. 3 (1993): 189–98. See also P. L. Gerbarg, “Yoga and Neuro-Psychoanalysis,” in Bodies in Treatment: The Unspoken Dimension, ed. Frances Sommer Anderson (New York, Analytic Press, 2008), 127–50.
13.D. Emerson and E. Hopper, Overcoming Trauma Through Yoga: Reclaiming Your Body (Berkeley, North Atlantic Books, 2011).
14.A. Damasio, The Feeling of What Happens: Body and Emotion in the Making of Consciousness (New York, Hartcourt, 1999).
15.“Interoception” is the scientific name for this basic self-sensing ability. Brain-imaging studies of traumatized people have repeatedly shown problems in the areas of the brain related to physical self-awareness, particularly an area called the insula. J. W. Hopper, et al., “Neural Correlates of Reexperiencing, Avoidance, and Dissociation in PTSD: Symptom Dimensions and Emotion Dysregulation in Responses to Script-Driven Trauma Imagery,” Journal of Traumatic Stress 20, no. 5 (2007): 713–25. See also I. A. Strigo, et al., “Neural Correlates of Altered Pain Response in Women with Posttraumatic Stress Disorder from Intimate Partner Violence,” Biological Psychiatry 68, no. 5 (2010): 442–50; G. A. Fonzo, et al., “Exaggerated and Disconnected Insular-Amygdalar Blood Oxygenation Level-Dependent Response to Threat-Related Emotional Faces in Women with Intimate-Partner Violence Posttraumatic Stress Disorder,” Biological Psychiatry 68, no. 5 (2010): 433–41; P. A. Frewen, et al., “Social Emotions and Emotional Valence During Imagery in Women with PTSD: Affective and Neural Correlates,” Psychological Trauma: Theory, Research, Practice, and Policy 2, no. 2 (2010): 145–57; K. Felmingham, et al., “Dissociative Responses to Conscious and Non-conscious Fear Impact Underlying Brain Function in Posttraumatic Stress Disorder,” Psychological Medicine 38, no. 12 (2008): 1771–80; A. N. Simmons, et al., “Functional Activation and Neural Networks in Women with Posttraumatic Stress Disorder Related to Intimate Partner Violence,” Biological Psychiatry 64, no. 8 (2008): 681–90; R. J. L. Lindauer, et al., “Effects of Psychotherapy on Regional Cerebral Blood Flow During Trauma Imagery in Patients with Posttraumatic Stress Disorder: A Randomized Clinical Trial,” Psychological Medicine 38, no. 4 (2008): 543–54 and A. Etkin and T. D. Wager, “Functional Neuroimaging of Anxiety: A Meta-Analysis of Emotional Processing in PTSD,
Social Anxiety Disorder, and Specific Phobia,” American Journal of Psychiatry 164, no. 10 (2007): 1476–88.
16.J. C. Nemiah and P. E. Sifneos, “Psychosomatic Illness: A Problem in Communication,” Psychotherapy and Psychosomatics 18, no. 1–6 (1970): 154–60. See also G. J. Taylor, R. M. Bagby, and J. D. A. Parker, Disorders of Affect Regulation: Alexithymia in Medical and Psychiatric Illness (Cambridge: Cambridge University Press, 1997).
17.A. R. Damásio, The Feeling of What Happens: Body and Emotion and the Making of Consciousness (Random House, 2000), 28.
18.B. A. van der Kolk, “Clinical Implications of Neuroscience Research in PTSD,” Annals of the New York Academy of Sciences 1071, no. 1 (2006): 277–93. See also B. K. Hölzel, et al., “How Does Mindfulness Meditation Work? Proposing Mechanisms of Action from a Conceptual and Neural Perspective,” Perspectives on Psychological Science 6, no. 6 (2011): 537–59.
19.B. K. Hölzel, et al., “Mindfulness Practice Leads to Increases in Regional Brain Gray Matter Density,” Psychiatry Research: Neuroimaging 191, no. 1 (2011): 36–43. See also B. K. Hölzel, et al., “Stress Reduction Correlates with Structural Changes in the Amygdala,” Social Cognitive and Affective Neuroscience 5, no. 1 (2010): 11–17; and S. W. Lazar, et al., “Meditation Experience Is Associated with Increased Cortical Thickness,” NeuroReport 16 (2005): 1893–97.

